Short Dive: Fix Your Skin at the Root: Heal Your Barrier First (Part 1)
Why your skin feels sensitive, dry, oily, or breaking out and exactly how to repair your barrier for calm, glowy skin again.
She had good skin most of her life.
Nothing dramatic — just normal, unremarkable skin that she never thought about much. Then she turned 19, discovered skincare, and decided to actually take care of it.
She did everything she’d been taught to do on the internet. Double cleansed. Used a vitamin C serum in the morning. Introduced a glycolic acid toner. Added retinol at night because everyone said she should start young. Exfoliated twice a week. She had a ten-step routine and an entire shelf of products she’d carefully researched.
And her skin got worse.
Not a little worse. Noticeably, confusingly worse. She was doing more than she’d ever done for it, spending more money than she ever had, paying more attention than she ever had and her skin was redder, more reactive, breaking out in places it never had before, and stinging when she applied her moisturiser.
She went to a dermatologist. The verdict: her skin barrier was damaged. Not by neglect. By too much. By the very routine she’d built to help.
This is happening to a generation of women.
A 2024 survey by the International Dermal Institute found that 68% of dermatologists had treated patients in the last year for adverse reactions — contact dermatitis, severe purging, or barrier damage, linked to products or techniques popularised online. Not from using bad products. From using the right products in the wrong quantities, at the wrong time, in the wrong combinations, based on advice from people whose skin is different from theirs, who are paid to recommend things, and who are not dermatologists.
For years, the dominant logic of skincare was “more is better” — acids, peels, exfoliating toners, and masks layered together in pursuit of brighter, smoother skin. While these products delivered short-term results, the long-term impact was compromised skin barriers, chronic sensitivity, breakouts, and inflammation.
If you have skin that’s suddenly become reactive, that stings when you apply things it used to tolerate, that’s dry and oily at the same time, that breaks out more than it did when you were doing nothing — this might be why. And the fix is almost certainly the opposite of what the algorithm will tell you to try next.
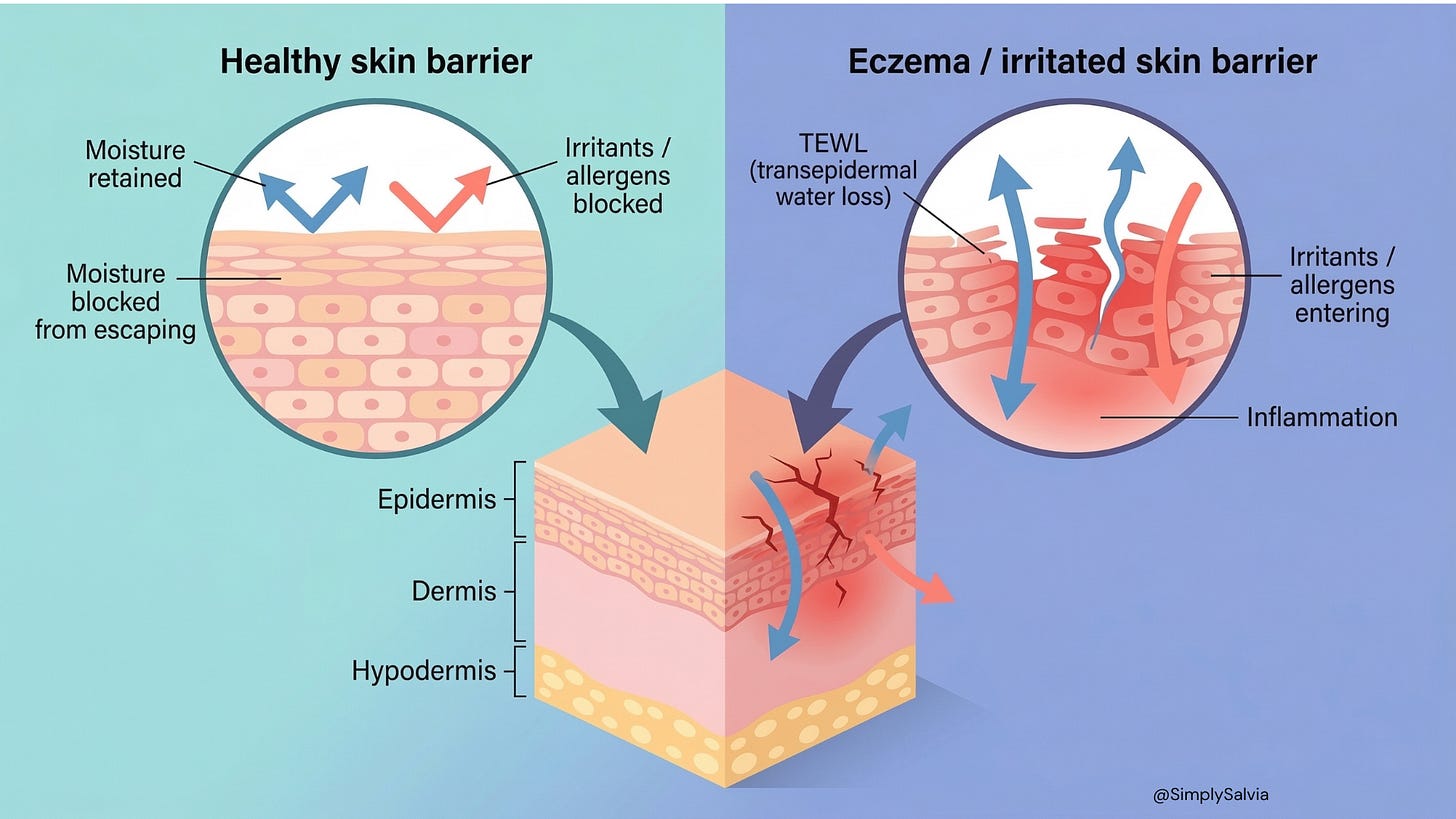
Here’s what nobody explains clearly enough: your skin barrier is not just a cosmetic concern. It is a physical structure, a carefully maintained layer of cells and lipids and microbes that your body has been building and maintaining your entire life. It keeps water inside your skin and keeps pathogens, allergens, and irritants out. Your skin functions as an active immune organ that blocks pathogens and initiates immune responses. Keratinocytes — the cells that form your skin’s outer layer, act as biological alarm systems. When they detect danger, they release antimicrobial peptides and signalling molecules that alert your immune system.
When that barrier is intact, your skin is comfortable, hydrated, and resilient. When it’s damaged, everything you put on it goes where it’s not supposed to go. Actives that were designed to sit on the surface penetrate too deeply. Moisture evaporates faster than it can be replaced. Irritants get in. Your immune system activates in response to things it would normally ignore. Skin that used to be “normal” becomes “sensitive” not because your skin type changed, but because the structural layer that was protecting it has been thinned, stripped, and disrupted.
And it is very easy to damage it, because the tools that damage it are being marketed to you specifically as skincare.
I started looking into this properly because I noticed a pattern. So many women I know, and so many in the comments of the skin content I watch, describe the same trajectory: started taking skincare seriously, built a routine, saw initial improvement, then hit a wall where nothing seemed to work and everything seemed to make things worse. The assumption is usually that their skin needs something stronger. A new acid. A higher concentration retinol. A different routine.
The research says the opposite. The skincare industry is now seeing a clear shift away from the “more is better” mindset. Over-exfoliation, compromised skin barriers, and sensitised complexions have pushed both brands and consumers to reassess what healthy skin actually looks like. The answer is moderation and precision — fewer products, better ones, applied in ways that respect the skin’s natural biology.
This Short Dive is about what the skin barrier actually is, why it’s breaking down in women our age in particular, and what the evidence says about repairing it — from both the outside and the inside.
Here’s what this Short Dive covers:
What the skin barrier actually is — the science, in plain language
How to tell if yours is damaged
The most common ways it gets damaged — and the skincare habits most likely to be the culprit
Different types of barrier disruption and why they need different approaches
What to eat, how to sleep, and how to manage stress to rebuild from within
The ingredients that actually repair it — and what to avoid while it heals
A gentle 7-day reset routine to get you started
The 19-year-old with the ten-step routine has simpler skin now than she did when she started. Not because she found better products. Because she stopped using most of them.
Let’s get into it.
Hope you enjoy reading and learning with me, Simply Salvia
PS: We also have a subscriber-only group chat where members discuss the deep dives, share their sleep journeys, and ask me questions directly. See you there.
Disclaimer: The information and opinions expressed above are current as of the date of this post and are subject to change without notice. Materials referenced above are provided for educational and informational purposes only. None of the above constitutes medical advice, a diagnosis, a treatment recommendation, or a substitute for consultation with a qualified healthcare professional. Always seek the guidance of your doctor or another qualified health provider with any questions you may have regarding a medical condition or sleep disorder.
Short Dive below ↓
Dry, Reactive, or Breaking Out? How to Diagnose Your Barrier Type
Feed Your Barrier: The Nutrients That Rebuild Your Skin From the Inside Out
The Daily Habits That Either Protect or Destroy Your Skin Barrier (Most People Get These Wrong)
Which Supplements Actually Help Your Skin Barrier — And the Doses That Make a Difference
The Kitchen Remedies and Herbal Teas That Calm, Repair, and Rebuild Your Barrier
The Barrier Rescue Routine: Exactly What to Use, In What Order, And What to Stop Immediately
Chapter 1: What Is the Skin Barrier?
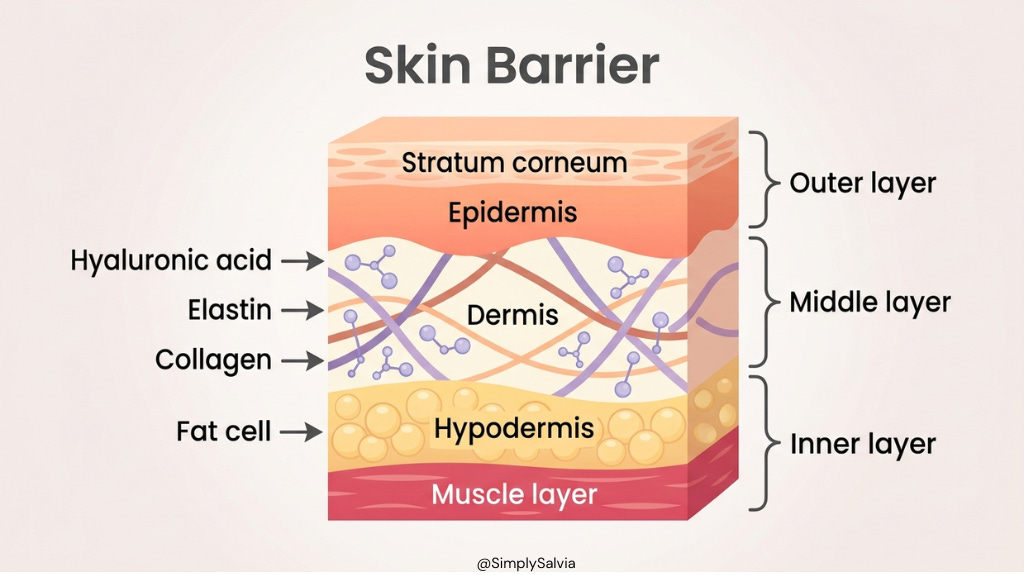
If your skin keeps reacting no matter what you try — new products, gentle routines, more water. The problem probably isn’t your products. It’s the barrier underneath them. Before we fix it, let’s understand it. The skin is composed of multiple layers, but the “skin barrier” mainly refers to the outermost layer of the epidermis called the stratum corneum. This layer is extremely thin (think cellophane thickness) but tough. As mentioned, you can visualize it as bricks and mortar. The bricks are dead, flattened skin cells (corneocytes) that are rich in keratin and natural moisturizing factors. The mortar between them is a lipid matrix made up of fatty substances; ceramides (about 50%), cholesterol (about 25%), and fatty acids (about 25%). These lipids form structured layers around the cells, creating a water-resistant seal.
Together, this structure has two main jobs:
Keep bad stuff out (irritants, bacteria, allergens, pollutants)
Keep good stuff in (moisture especially)
When healthy, the barrier is selectively permeable. It lets in small beneficial molecules (like water and certain skincare ingredients) but blocks large or harmful ones. It’s amazingly effective: an intact barrier prevents most microbes and chemicals from penetrating, while holding onto natural hydration so our skin doesn’t constantly lose water.
Not only that, the barrier layer helps maintain skin’s immune balance. The surface is slightly acidic (pH around 5) which inhibits harmful bacteria and supports the skin microbiome. The collection of friendly microbes living on us. (Yes, we have good bacteria on our skin that act as microscopic bodyguards!) A healthy microbiome further crowds out pathogens and even “talks” to our skin’s immune cells to keep inflammation in check. In essence, your skin barrier isn’t just passive wall – it’s an active defense system, complete with its own ecosystem and alarm signals when breached.
Key barrier functions include:
Moisture Retention
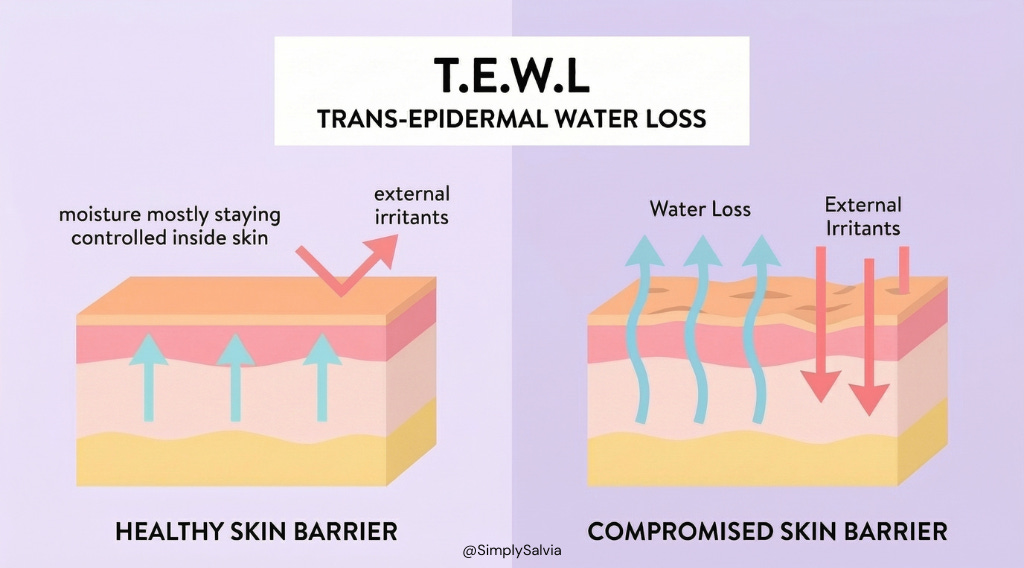
The lipid “mortar” is hydrophobic, meaning it repels water. This prevents transepidermal water loss (TEWL) water evaporating from deeper skin. A strong barrier keeps your skin hydrated and plump. When the barrier is leaky, you get dryness and that annoying tight feeling. In fact, ceramides and cholesterol in the barrier are crucial to preventing moisture from evaporating.
Protection Against Outsiders
A healthy barrier is like a shield. It blocks toxins, pollutants, and germs from penetrating your skin. Those tightly packed bricks and lipids are very selective. For example, ceramides fill the gaps so well that they inhibit the penetration of foreign pathogens or allergens. This protects you from infections and irritation.
Immune Regulation
The barrier also contains specialized cells and signals (like antimicrobial peptides, cytokines) that trigger immune responses when needed. If something breaches the barrier, alarm chemicals signal deeper skin to react (sometimes seen as redness or inflammation). Also, the acidic pH and friendly bacteria on the surface are part of immune defense, they create an environment that deters harmful bugs and educates your immune system not to overreact to every little thing. When the barrier is intact, it helps calm the skin’s immune responses; when broken, the immune system can go into overdrive leading to conditions like eczema, where a broken barrier and inflammation feed each other.
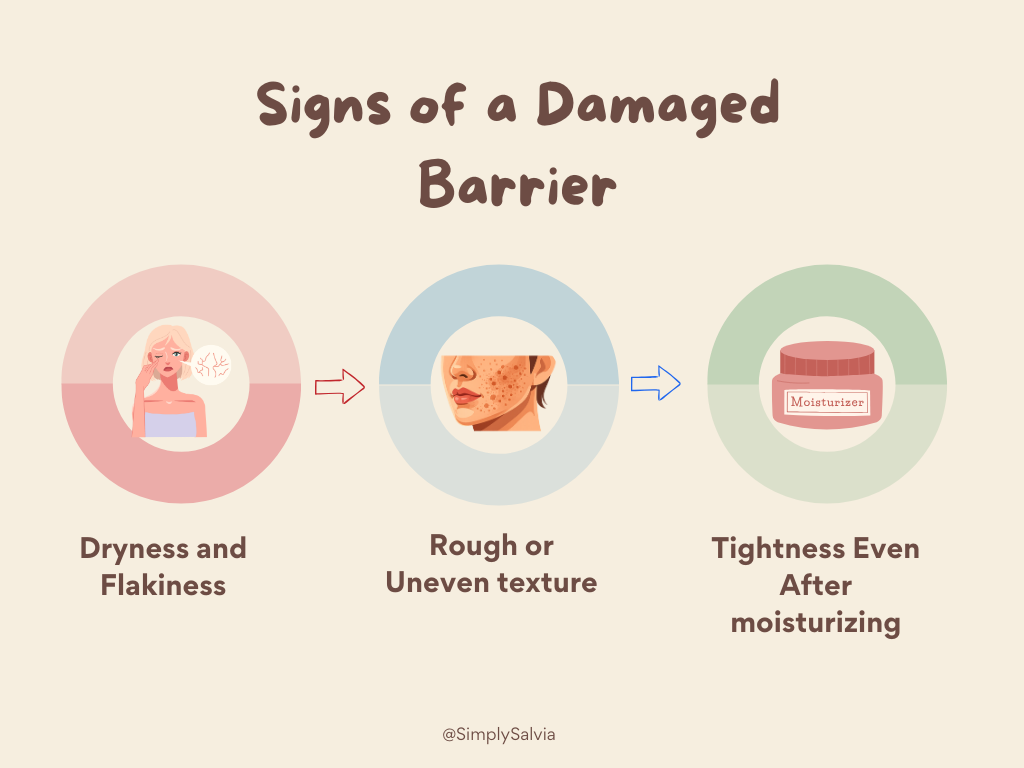
Signs of a Damaged Barrier
How do you know if your skin’s barrier is compromised? Your skin will tell you. Common signs include:
You might see redness or feel itching, burning or stinging when you apply products whereas healthy skin wouldn’t react so strongly. Breakouts or rashes can occur because irritants and bacteria sneak in through the “cracks,” leading to pimples or irritant dermatitis. In fact, a damaged barrier often underlies adult acne or “sensitive” skin complaints as your skin becomes reactive because its shield is down. You may notice your skin is less plump and more dull, since it’s losing water and struggling to reflect light well. In summary, compromised barrier skin tends to be dry, reactive, red, and prone to breakouts or infections. If this sounds familiar, don’t worry – it’s fixable, and you’re in the right place to learn how.
Chapter 2: Why Skin Barrier Damage Happens
Now let’s explore what causes the barrier to break down. It usually isn’t just one thing rather its often a combination of factors slowly (or sometimes suddenly) wears away at that protective layer. Lets look at external triggers from skincare routines, and internal or environmental factors that weaken the barrier.
Skincare Triggers: Doing “Too Much”
Ironically, many barrier problems are self-inflicted by our well-intentioned skincare habits. In the quest for perfect skin, it’s easy to overdo it and strip or irritate the barrier. Some common culprits:
Over-cleansing: Washing your face too often or with harsh cleansers can deplete the natural oils and disturb the acidic pH of your skin. Foaming cleansers with sulfates or alcohol-based astringents are especially guilty. They give that “squeaky clean” feeling which is actually your barrier being stripped. Over-cleansing (more than twice a day) or using strong soaps can weaken the mortar between skin cells.
Harsh toners and alcohol: That bracing tingle from an alcohol-heavy toner might feel effective, but it often means your barrier is getting degreased. Denatured alcohol and witch hazel-based toners can overly dry out the stratum corneum, leading to microscopic cracks and water loss. If your skin feels tight or “shiny-dry” after toning, it’s a red flag. Opt for hydrating, alcohol-free toners instead.
Excessive exfoliation: This is a big one. Exfoliants are useful in moderation to remove dead cells, but many of us have taken exfoliating to extremes with daily acids, peels, scrubs, and microdermabrasion. Alpha-hydroxy acids (AHAs), beta-hydroxy acids (BHAs), and scrubs can thin the stratum corneum if overused, eroding that protective brick wall. The result? Skin that’s smooth at first, then chronically irritated and prone to stinging and redness. Over-exfoliation basically sands away your mortar. Dermatologists often see patients with red, shiny, sensitive skin from using multiple exfoliating products at once. If your skin is inflamed, dial it way back on these.
Strong actives without support: Potent ingredients like retinoids (retinol, tretinoin), benzoyl peroxide, high-percentage vitamin C or glycolic acid can transform skin but they also can cause barrier damage if used too aggressively. Retinoids in particular speed up cell turnover, which can cause peeling and microscopic barrier gaps (sometimes called the “retinol uglies” or “purge” at the start). Using these actives without moisturizing adequately or introducing them too fast is a recipe for a compromised barrier.
Fragrance and preservatives in products can also trigger irritation in some people, further inflaming the skin. It’s not that these actives are “bad” it’s about how you use them. More on this in the routine chapter.
In short, the modern 10-step routine can backfire. When we bombard our skin with too many products – cleansers, peels, toners, serums, spot treatments, etc. we risk damaging the very barrier we’re trying to beautify. Simpler and gentler is often better for barrier health.
Internal & Environmental Factors: The Less Obvious Causes
It’s not only about skincare products. Lifestyle and environment play a huge role in skin barrier integrity:
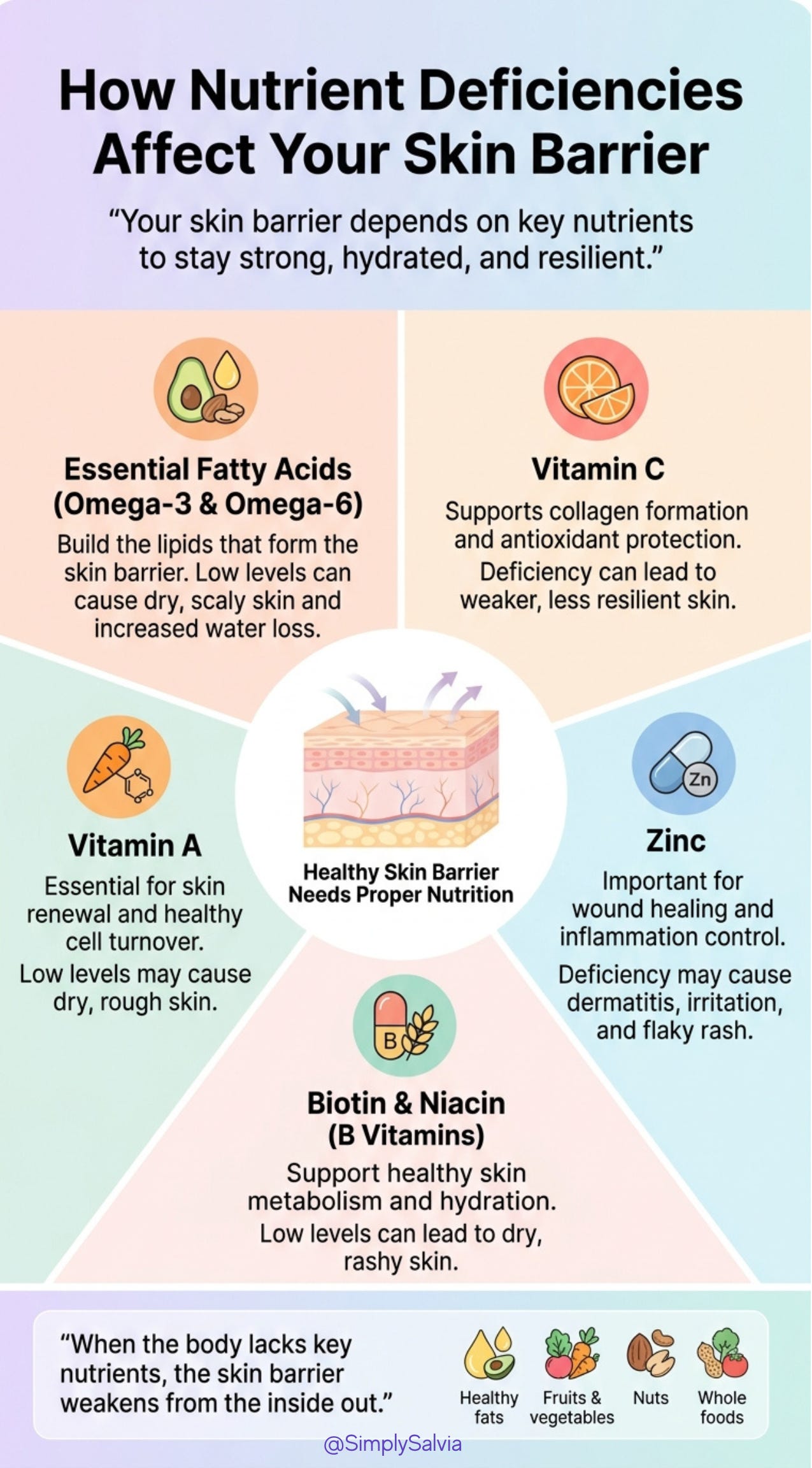
Poor nutrition or deficiencies: Your skin barrier needs certain nutrients as building blocks. For example, essential fatty acids (EFAs) like omega-6 and omega-3 are needed to produce the lipids (ceramides, etc.) in the stratum corneum. A diet very low in healthy fats can lead to dry, scaly skin and in extreme cases, an EFA deficiency causes eczema-like dermatitis with increased water loss.
Vitamin C and Vitamin A are crucial for skin renewal; a lack of vitamin C impairs collagen formation and antioxidant defense, potentially leaving skin dehydrated and less resilient.
Zinc is vital for wound healing and controlling inflammation, so low zinc can manifest as rough, easily irritated skin. In fact, a zinc deficiency is known to cause dermatitis and flaky rash in severe cases.
Biotin (vitamin B7) and niacin (B3) are also important and deficiencies can cause dry, rashy skin. The bottom line: if your body is missing key nutrients, your skin barrier may weaken from the inside out. (I’ll dive deeper into diet in Chapter 4.)
Dehydration: Not drinking enough fluids or losing too much (think intense exercise without rehydrating, or just living in a dry climate and forgetting to hydrate) can leave your skin poorly hydrated. When your body is dehydrated, skin cells don’t have the water content they need, and the barrier becomes more brittle. In fact, chronic dehydration is associated with reduced skin elasticity and a compromised barrier, essentially accelerating skin aging and fine lines. If you notice your skin looking dull and “crêpey,” ask if you’ve been drinking enough water.
Tip: also check if you’re overdoing the caffeine or alcohol, which can dehydrate.
Lack of sleep & disrupted circadian rhythm: Beauty sleep is a real thing. During deep sleep, your skin goes into repair mode – blood flow increases, and the barrier undergoes renewal and barrier lipids get replenished. If you’re chronically short on sleep, those repair processes may lag. Studies have shown sleep deprivation delays skin barrier recovery after irritation, basically, skin heals slower. Ever notice how a bad night’s sleep can leave your face looking dull or more inflamed? Over time, poor sleep correlates with more signs of skin aging and unevenness. Strive for a consistent 7–8 hours; your skin uses that time wisely!
Chronic stress & high cortisol: Stress isn’t just in your head, it shows up on your skin. When you’re under psychological stress, your body releases cortisol (the stress hormone), which can impair skin’s barrier function. High cortisol can increase transepidermal water loss and delay barrier recovery. In one study, stressed individuals had significantly higher TEWL (water loss) and a weaker skin barrier compared to relaxed individuals. Have you ever gotten an eczema flare or breakout during a stressful week? That’s no coincidence, stress-induced barrier disruption plus inflammation is likely at play. Managing stress (through breathing, meditation, exercise, etc.) can actually improve your skin’s resilience. Think of stress as acid rain on your skin’s brick wall; over time it erodes the structure unless neutralized.
Sun exposure (UV radiation): Excess unprotected sun is a major barrier saboteur. UV rays generate free radicals in the skin that damage cells and lipids. A sunburn is an acute example of barrier destruction. The red, peeling skin is essentially a compromised barrier that has to rebuild itself. Even low-level daily UV exposure depletes ceramides and causes inflammation. Always protect your skin with sunscreen, hats, etc. to minimize this. UV also ages the skin by breaking down collagen, another reason to shield yourself.
Pollution and environmental toxins: City dwellers, take note – air pollution like particulate matter, smoke, smog can cling to skin and generate oxidative stress, which inflames and weakens the barrier. Pollutants can disrupt the skin microbiome balance as well. It’s been observed that people in high-pollution areas have higher rates of eczema and irritation. While you can’t avoid air quality entirely, gentle cleansing at night to remove pollutant particles and using antioxidants can help counter this.
Climate: cold, wind, and low humidity: Dry climates or winter weather are notorious for causing “winter itch” or dry, flaky skin. That’s because low humidity air draws moisture out from the skin. Cold temperatures also reduce skin’s natural oil production. The result is a dried-out mortar between your skin cells. Indoor heating in winter compounds this by creating desert-like air in homes. Likewise, strong wind can physically abrade and strip the skin’s oils (ever had windburn on your face?). To combat this, you need to add extra moisture and occlusion like heavier creams, in such conditions and use humidifiers indoors.
Age and genetics: Our barrier naturally changes with age. After age 40, skin produces fewer lipids. Studies show ceramide levels in the stratum corneum drop by over 30% as we hit middle age. Less mortar means more dryness and slower barrier repair. This is why mature skin often leans dry and sensitive. Additionally, some people inherit a tendency for weaker barrier. For example, individuals with eczema (atopic dermatitis) often have a genetic mutation in the filaggrin gene (FLG). Filaggrin is a protein crucial for forming the skin barrier; if it’s deficient, the barrier is “leaky.” A loss-of-function mutation in FLG leads to reduced filaggrin and a skin barrier defect, contributing to the chronic dryness and inflammation seen in eczema. Psoriasis is another condition where the barrier is disrupted as part of the disease process. Even without a diagnosed disorder, some people are simply born with more delicate skin that needs extra care, if you know your skin is reactive from childhood, you might be one of them.
It’s often a combination of these factors that lead to barrier woes. For instance, you might be using a harsh foaming cleanser (skincare trigger) and living in a low-humidity environment and not getting enough omega-3s. A perfect storm for a damaged barrier. The empowering part is that many of these factors are modifiable. By adjusting your routine and habits, you can remove the causes and let your skin rebuild.
Before we jump to solutions, let’s identify what kind of barrier damage you might have, since that can guide the approach.
Chapter 3: Dry, Reactive, or Breaking Out? How to
Diagnose Your Barrier Type
Not all barrier problems are identical. Your skin could be lipid-depleted (lacking oils), microbiome-disrupted, inflamed, or a mix of all. Identifying the primary type of barrier impairment can help you target the fix. Here are a few types and their clues:
Lipid Barrier Disruption
This is when the “mortar” between your skin cells is deficient or damaged.
Essentially, without enough lipids, your skin can’t hold water. It literally loses moisture to the air and becomes rough. If your face ever feels paper-thin and crinkly, that’s it. This type often comes with increased sensitivity too, because cracks in the mortar let irritants in easily. Restoring lost ceramides and oils is key here. In fact, studies show that a drop in ceramide levels directly causes dry, barrier-disrupted skin. Think of this type as “desert skin” parched and in need of moisture and fats.
Microbiome Imbalance (Dysbiosis)
Sometimes the issue isn’t lack of lipids, but rather an imbalance in the skin’s microbial flora. We co-exist with millions of bacteria on our skin. If the “good” bacteria get wiped out say by harsh antiseptics, overuse of antibiotics or certain preservatives or the environment changes (pH rises, barrier lipids change), bad microbes can overgrow.
Clues: This often shows up as inflammation – redness, little bumps or pimples, and even breakouts. You might not be dry; in fact, areas could be oily or have clogged pores since some bacteria like C. acnes flourish and trigger acne. Or you might experience unexplained rashes or itching. Dysbiosis can also exacerbate conditions like eczema or rosacea.
Typical scenario: you over-cleansed with harsh soap, stripping your acid mantle and killing many commensal (good) bacteria, now your skin is red, broken out, and anything you apply stings. People often misattribute it to an allergic reaction, but it can be a microbiome issue. Research shows an imbalanced microbiome can lead to redness, itchiness or dryness as common symptoms. To fix this type, you focus on gentle products that support the microbiome (proper pH, possibly probiotic skincare) and avoid antibacterial overkill. Skin might also benefit from fermented ingredients or lactic acid, which lower pH to a healthy range for good flora.
Inflammatory Barrier Damage
In some cases, the barrier is acutely inflamed due to a trigger that caused irritation for example, you had an allergic reaction to a fragrance, or you did a too-strong chemical peel. Here the issue isn’t just lack of oils or microbes, but that the skin is angry.
Clues: Burning, redness, heat, and swelling are obvious signs of inflammation. The skin may be less dry and more irritated e.g. it turns red and stings when you apply even simple products like sunscreen. There could be a rashy texture.
This type often overlaps with the others for instance, once lipids are stripped, inflammation follows. But it’s characterized by that irritation sensation; a feeling that your skin is “hot” or prickly. If you have rosacea or allergic eczema, you know this feeling well. In acute cases, you might recall a specific event:
I left a strong AHA mask on too long and my face has been burning since.
Immune cells are in overdrive and the barrier integrity is compromised, leading to nerve exposure (ouch). The focus here is on soothing and calming the inflammation first, then restoring moisture. Think cool compresses, anti-inflammatory botanicals (like colloidal oatmeal or aloe). Once the redness subsides, you’ll likely notice dryness and can address barrier lipids.
Combination Types
Often, these conditions overlap. For example, someone with eczema has a genetic lipid barrier weakness and often dysbiosis and inflammation. Acne-prone individuals might have a disturbed barrier, sometimes from harsh acne treatments, plus microbial imbalance with C. acnes bacteria plus inflammation. If you’ve ever used too many actives, you might get the trifecta: dry flakes, breakouts, and redness altogether. Don’t be overwhelmed though as the approach in such cases is a holistic one: gently restore moisture, rebalance the flora, and calm the skin. Luckily, many remedies like proper moisturizers and probiotics address multiple issues at once.
How can you differentiate?
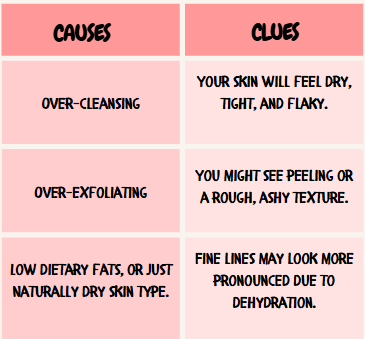
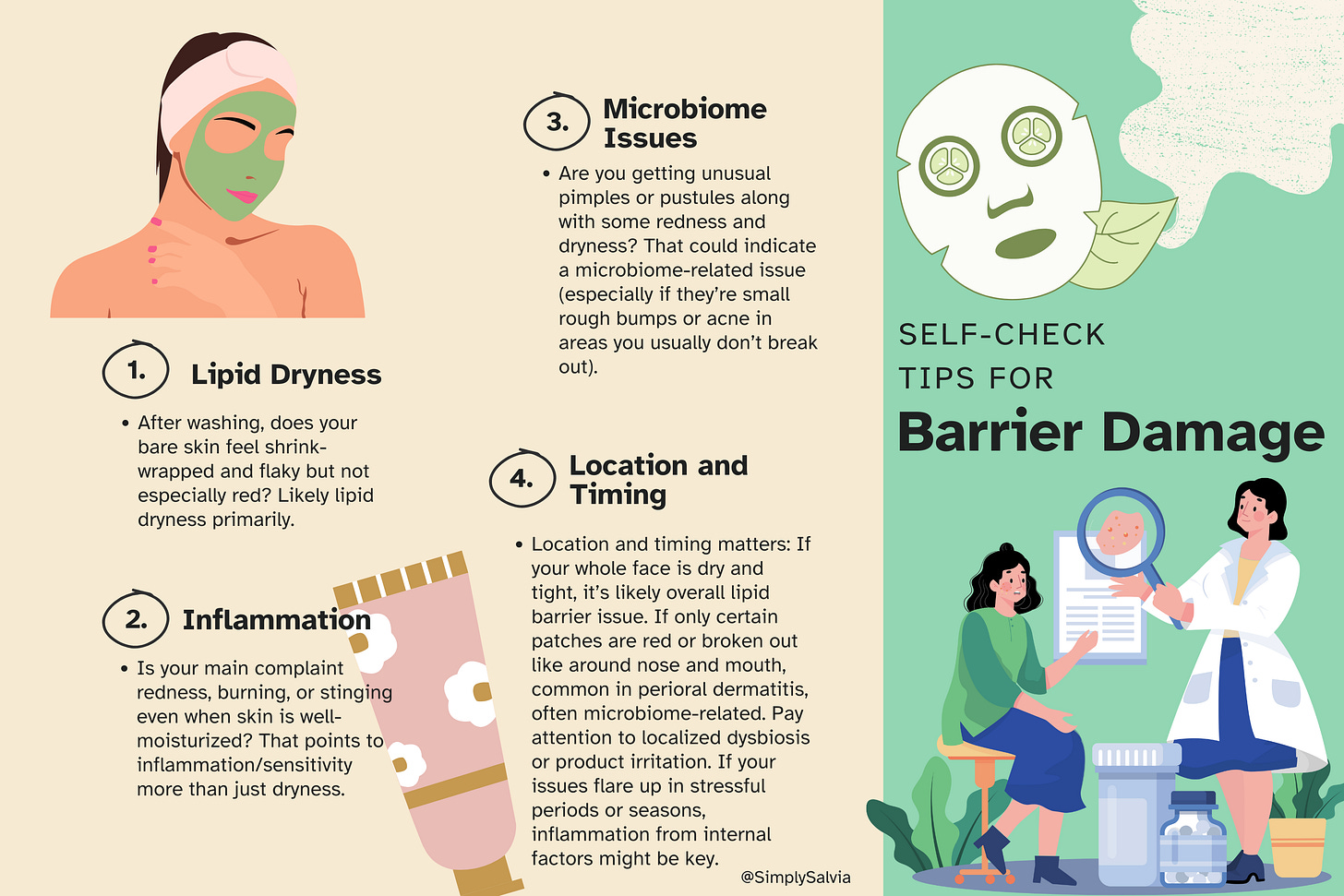
Here are a few self-check tips:
In practice, the strategies to fix these overlap a lot because the goal is to restore balance in all aspects. But identifying the dominant issue helps. For instance, if you conclude “I’ve just over-exfoliated, my skin is parched but not super red,” you’ll lean heavily into replenishing oils and humectants. If instead “My face is on fire after a reaction,” you’ll first use calming soaks and balms to bring the inflammation down. So take a moment to assess your own skin: is it crying out mainly from dryness, or from irritation, or both? Keep that in mind as we move into solutions.
Now you know what your barrier is, what’s been breaking it down, and which type of damage you’re dealing with. That’s already more than most skincare content will ever tell you. But knowing the problem is only half the journey. In Part 2, I go deep on the fix: what to eat to rebuild your barrier from the inside, the supplements worth taking (and the ones that aren’t), the herbal teas and DIY remedies that actually work, a complete daily routine, and the hormonal connection that explains why your skin behaves completely differently depending on where you are in your cycle. Part 2 is available to paid subscribers. If this post resonated, that’s your sign