Short Dive: Everyone’s Talking About ‘Cortisol Face’ — Most of It Is Wrong (Part 1)
The real science behind cortisol skin, minus the TikTok panic, the supplement industry spin, and the advice that treats your face like a problem to fix rather than a system to understand.
Your face has been trying to tell you something.
Maybe it’s the breakout that showed up two weeks after the most stressful month of your life — right when you thought you’d gotten through it. Maybe it’s the puffiness that’s taken up permanent residence under your eyes no matter how much sleep you get. The dullness that settles in during exam season and lifts, mysteriously, when you’re on holiday. The skin that used to tolerate everything and now stings when you put anything on it.
Or maybe you’ve seen the TikToks. The ones about cortisol face; the rounder jaw, the puffier cheeks, the idea that your stress hormones are physically redistributing fat in your face. And you’ve looked in the mirror and wondered: is that what’s happening to me?
The honest answer is: maybe. But probably not in the way the algorithm is describing it.
In early 2024, the comedian Amy Schumer posted on Instagram that she’d been diagnosed with Cushing’s syndrome after people online made comments about her face looking different. It was a genuine diagnosis — a rare hormonal condition in which the body produces so much cortisol that it causes clinically measurable physical changes, including facial fat redistribution. The internet took this moment, stripped out the “rare hormonal condition” part, and turned it into a content category.
Now “cortisol face” is everywhere. Along with cortisol supplements, cortisol-lowering routines, cortisol morning protocols, and a general cultural anxiety about a hormone that, ironically, spikes in response to anxiety.
Here’s what I found when I actually went looking at the research: the relationship between cortisol and your skin is real, well-documented, and genuinely significant. But it’s not what most of the content describes. It’s more interesting than that and more actionable.
This Short Dive separates the three things that all get called “cortisol face.” It explains what cortisol actually does to your skin at the cellular level, because it’s more than just “stress causes breakouts.” It covers how to tell if stress is driving your skin symptoms, what diet and lifestyle changes the research supports, which supplements have real clinical evidence behind them, and how to build a routine that works with your cortisol rather than against it.
What’s covered:
Let’s get into it.
PS: We also have a subscriber-only group chat where members discuss the deep dives, share their sleep journeys, and ask me questions directly. See you there.
Disclaimer: The information and opinions expressed above are current as of the date of this post and are subject to change without notice. Materials referenced above are provided for educational and informational purposes only. None of the above constitutes medical advice, a diagnosis, a treatment recommendation, or a substitute for consultation with a qualified healthcare professional. Always seek the guidance of your doctor or another qualified health provider with any questions you may have regarding a medical condition or sleep disorder.
Short Dive below ↓
Table of Contents:
The Three Things People Call "Cortisol Face" (They Are Not the Same)
What Your Diet Is Doing to Your Cortisol Levels
Sleep, Exercise, and the HPA Axis
Supplements and Adaptogens — Honest Rankings
The Skincare Side: Building a Routine That Works With Your Cortisol, Not Against It
Your Cortisol Action Plan
What to Take Away From This
CHAPTER 1: What Is Cortisol, Actually?
The hormone everyone talks about, explained properly
Cortisol has a branding problem. It’s been positioned as the enemy. The stress hormone, the thing making you fat and anxious and spotty. The wellness industry has built an entire supplement category around “lowering” it, implying that less cortisol is always better and that you want your levels as low as possible.
Neither of those things is true. And understanding what cortisol actually does, and why you genuinely need it is the foundation for understanding what happens when it goes wrong.
What Cortisol Does (It’s Not Just Stress)
Cortisol is a steroid hormone produced by the adrenal glands, which sit just above your kidneys. It belongs to a class of hormones called glucocorticoids aka the hormones that regulate glucose metabolism, immune function, and inflammation throughout the body.
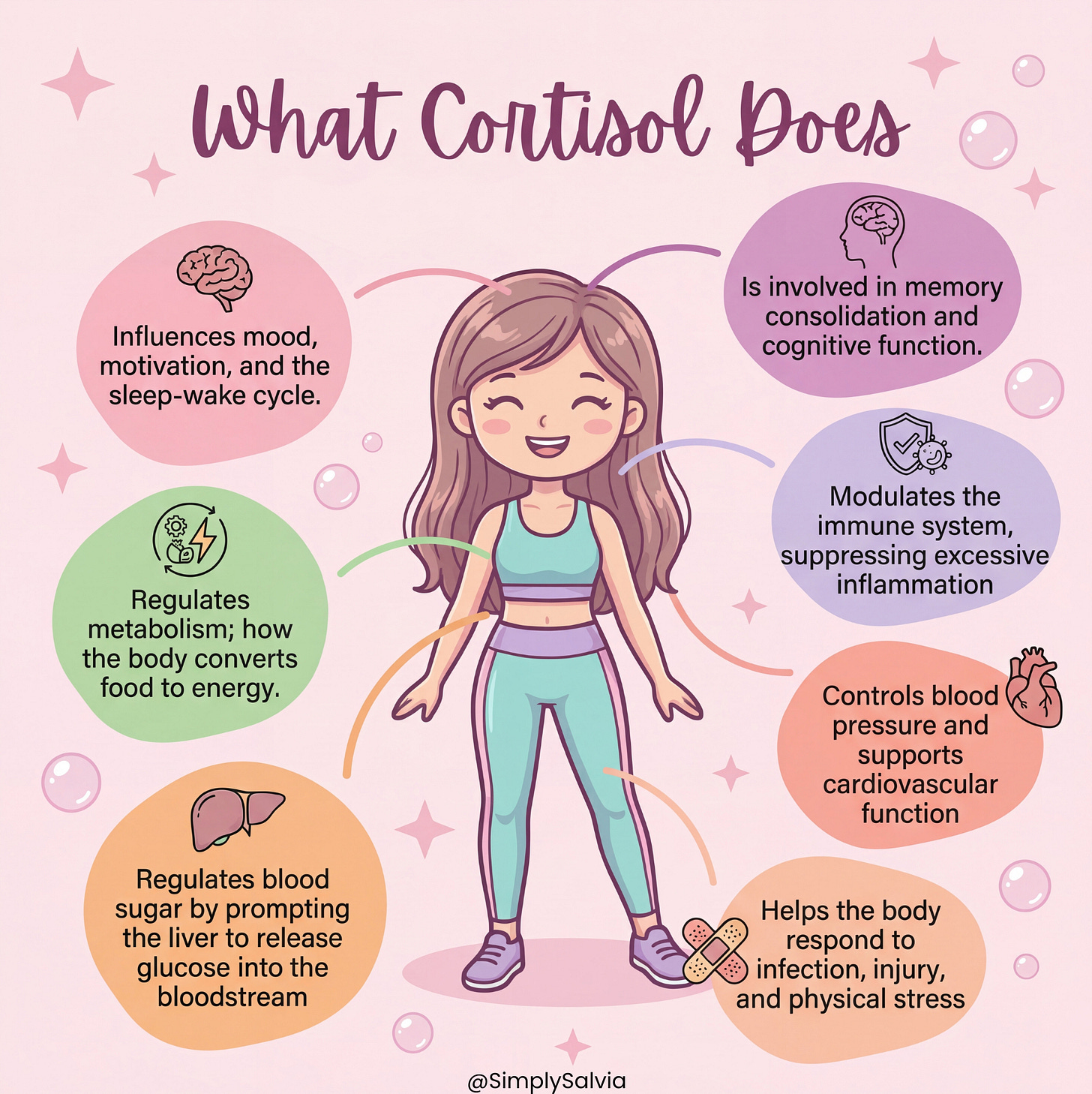
Its roles are extensive. Cortisol:
Regulates blood sugar by prompting the liver to release glucose into the bloodstream
Controls blood pressure and supports cardiovascular function
Modulates the immune system, suppressing excessive inflammation
Helps the body respond to infection, injury, and physical stress
Regulates metabolism; how the body converts food to energy
Is involved in memory consolidation and cognitive function
Influences mood, motivation, and the sleep-wake cycle
Without cortisol, the body cannot regulate inflammation or blood pressure effectively, deficiency is life-threatening. The goal is never “as low as possible.” The goal is a well-functioning cortisol rhythm: the right amount at the right times.
The HPA Axis: How Cortisol Is Made
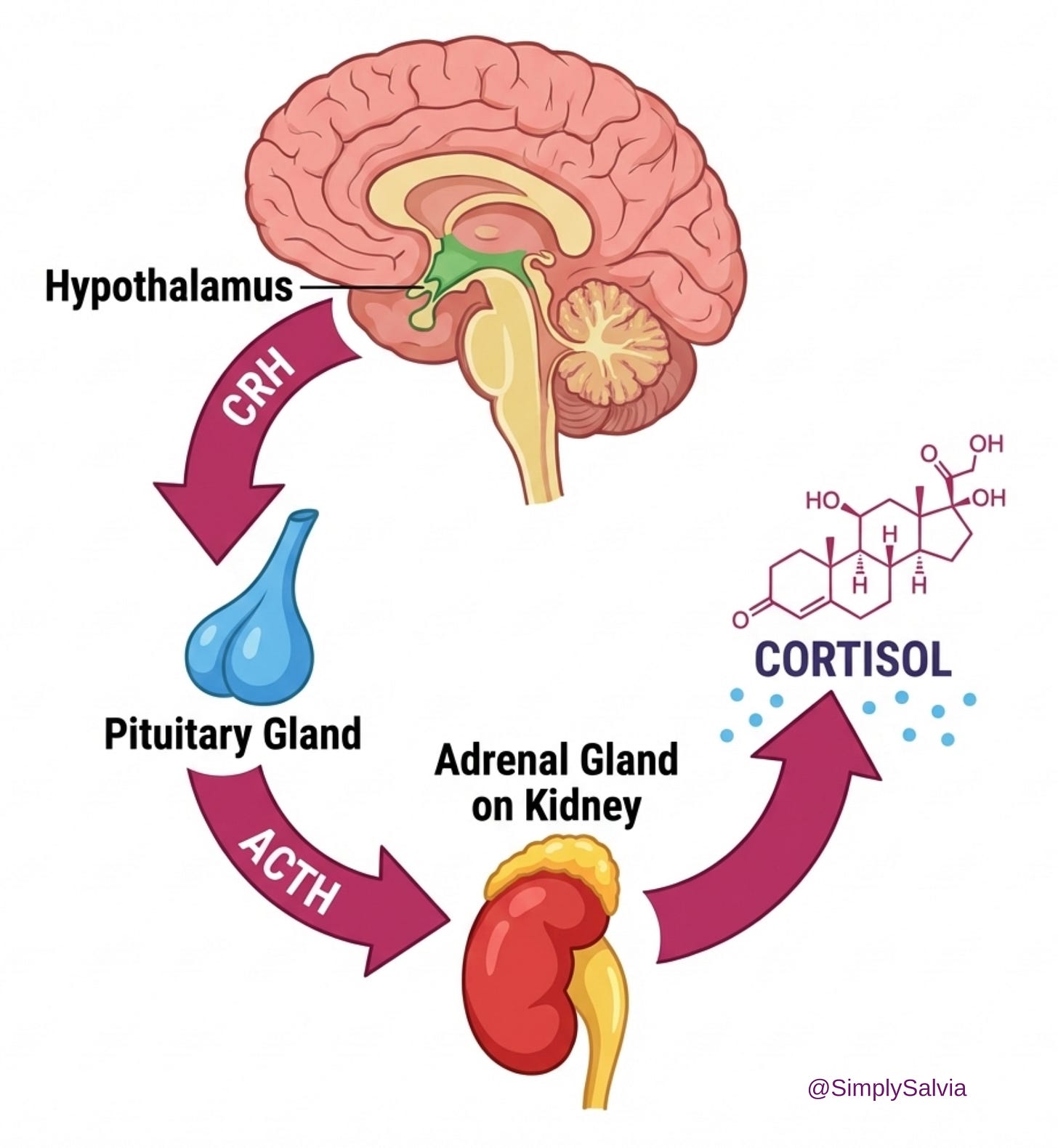
Cortisol production is controlled by a three-part communication system called the HPA axis — hypothalamus, pituitary, adrenal glands.
Here’s how it works: a stressor (physical, emotional, or perceived) activates the hypothalamus, which releases corticotropin-releasing hormone (CRH). CRH travels to the pituitary gland and signals it to release adrenocorticotropic hormone (ACTH). ACTH travels through the bloodstream to the adrenal glands and tells them to produce cortisol.
Once cortisol levels in the blood reach a certain point, the hypothalamus and pituitary detect this and reduce their signals — a negative feedback loop that normally keeps the system in balance. Chronic stress can disrupt this feedback sensitivity, leading to prolonged cortisol elevation and eventually reduced HPA axis responsiveness.
There’s also a separate system worth knowing about: the skin has its own peripheral HPA-like axis. Keratinocytes; the cells that make up your skin’s outer layer contain the components to produce cortisol locally. The skin doesn’t just respond to cortisol from the adrenal glands. It can produce it directly in response to local stressors like UV radiation, injury, and inflammation. This is why skin conditions can worsen with local stress even when systemic cortisol looks normal.
The Cortisol Rhythm: Why Timing Matters
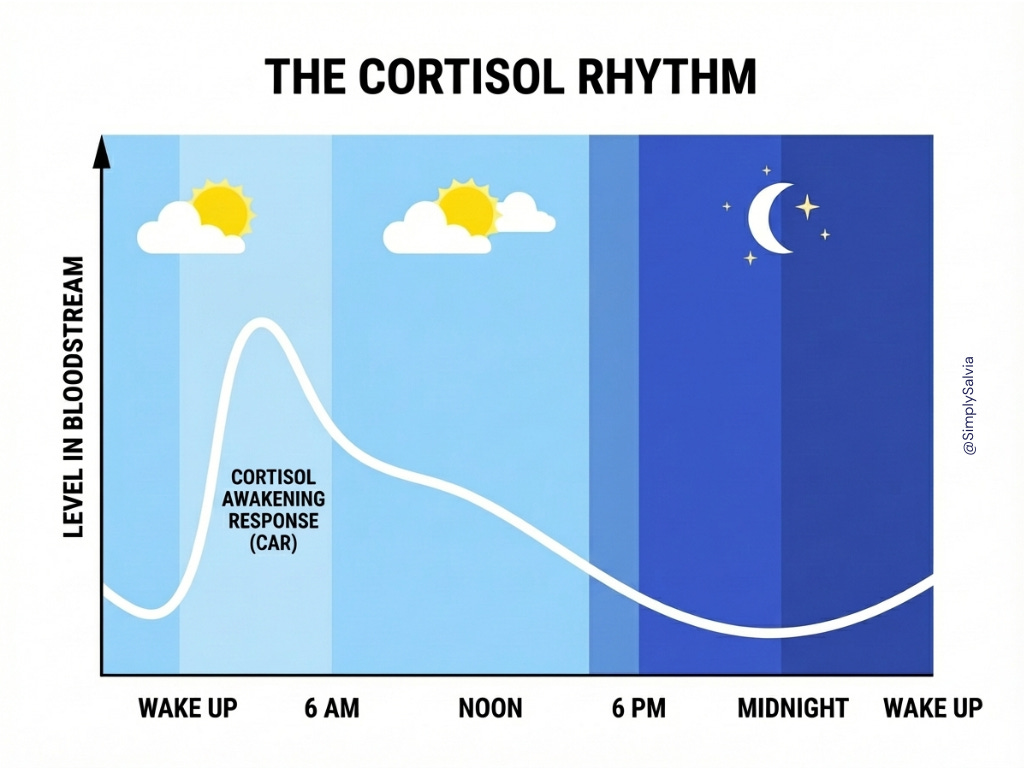
Cortisol is not supposed to be a steady flatline. It follows a diurnal rhythm: levels spike sharply in the 30 minutes after waking; a phenomenon called the cortisol awakening response (CAR), and then gradually decline throughout the day, reaching their lowest point around midnight.
This rhythm is essential. The morning cortisol surge mobilises energy, increases alertness, and primes the immune system for the day ahead. The evening drop allows the body to shift into repair and recovery mode, supports sleep onset, and permits the overnight processes that healthy skin depends on:
Cell turnover,
Collagen synthesis,
Immune regulation
When the rhythm is disrupted, by irregular sleep schedules, chronic stress, artificial light exposure at night, or extreme training, the consequences ripple through every system that cortisol touches. Including your skin.
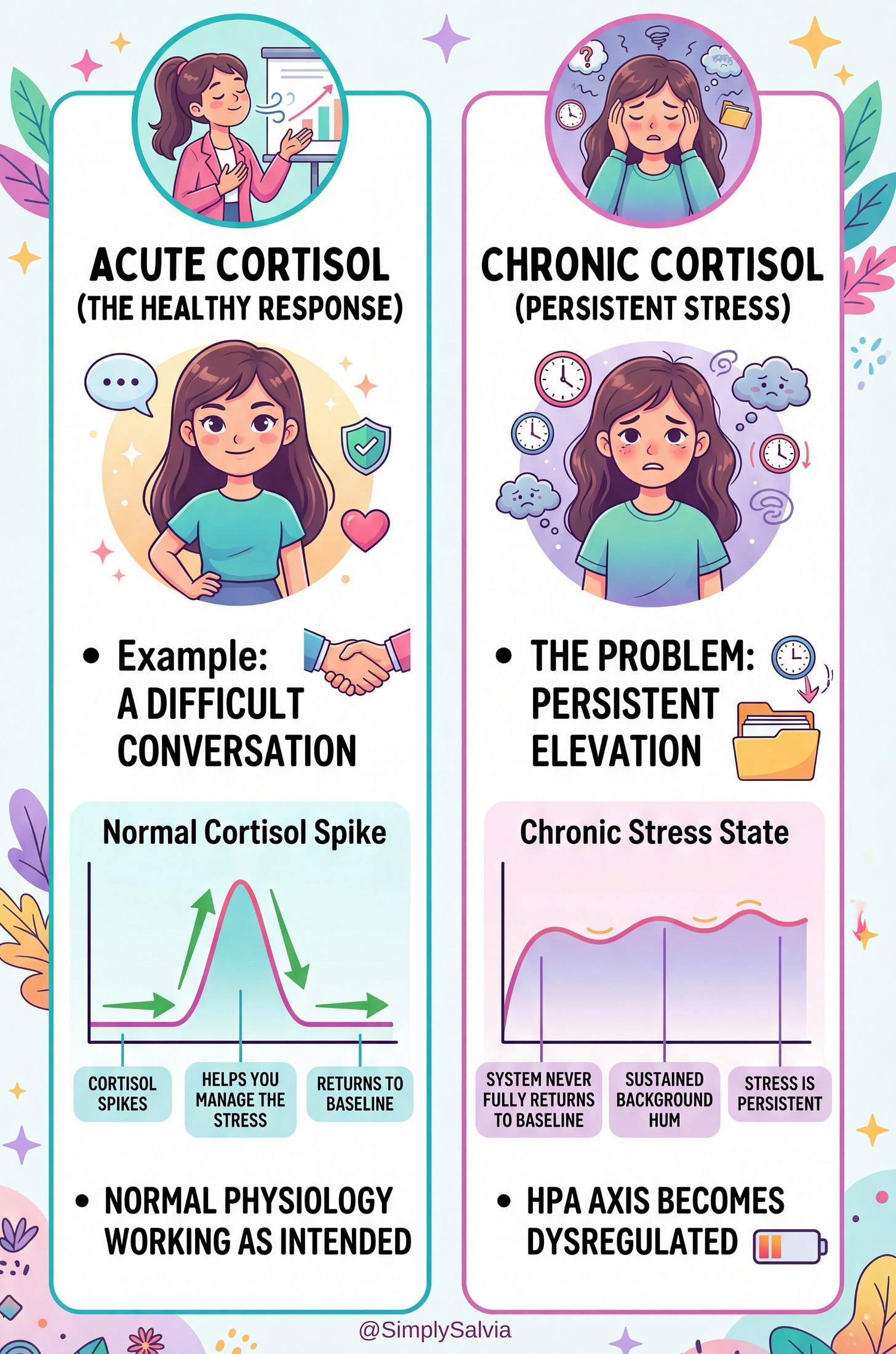
Acute vs. Chronic Cortisol: The Critical Difference
Acute cortisol responses are healthy. You have a difficult conversation; cortisol spikes, helps you manage the stress, then returns to baseline. This is normal physiology working as intended.
The problem is chronic elevation, when the system never fully returns to baseline. When the stress is persistent enough, or the HPA axis becomes dysregulated enough, cortisol stays elevated not in spikes but as a sustained background hum. This chronic moderate elevation is what the research consistently links to impaired skin barrier function, collagen breakdown, delayed wound healing, and increased sebum production.
And here’s the important point: you don’t have to feel dramatically stressed for this to be happening. Chronic low-level stress; the kind that comes from a relentless schedule, financial pressure, sleep deprivation, or just the baseline anxiety of being young and alive right now, can be enough to sustain mildly elevated cortisol long-term, with cumulative consequences for the skin.