Between Saturdays: What’s Actually Happening While You Sleep
From the brain circuit UC Berkeley just mapped that builds your muscle while you sleep, to why your gut microbiome is showing up on your face — four things from the research worth knowing about.
There’s a version of health advice that tells you what to do. And then there’s the version that explains why — the actual biology underneath the recommendation. The second version is harder to find and more useful once you have it. This week’s edition is heavy on the second version: why deep sleep is doing something most people don’t realise, why what you eat is showing up on your skin through a completely separate pathway than the one skincare talks about, why the research on exercise and mental health just got significantly stronger, and a finding about magnesium that’s specifically relevant for women.
Caught My Eye…
The Brain Circuit That Builds Your Muscle While You Sleep — UC Berkeley Just Mapped It
Most people know sleep is important. Fewer people know exactly why, in the specific, biological, this-is-the-mechanism sense. A study published in the journal Cell in September 2025 and summarised by ScienceDaily in March 2026 is one of the clearest answers yet, and it matters for anyone who exercises, anyone trying to change their body composition, and anyone who’s ever wondered why bad sleep makes everything harder.
Researchers at UC Berkeley mapped the neural circuits in the hypothalamus (the brain region that controls hunger, temperature, and hormone release) that control the release of growth hormone during sleep. What they found is that deep, non-REM sleep (the early, restorative phase of sleep that happens in the first few hours of the night) is the primary trigger for growth hormone surges. Not the only trigger, but the main one. And growth hormone is not just about growing taller as a teenager. In adults, it builds and repairs muscle tissue, strengthens bones, regulates fat distribution, supports blood sugar management, and plays a central role in metabolic health. Low levels are linked to muscle loss, belly fat accumulation, insulin resistance, and faster biological ageing.
The study also uncovered a feedback mechanism: as growth hormone builds up during sleep, it signals the brain region that controls alertness, which eventually pushes the body toward waking up. This explains why both too little sleep and disrupted sleep (the kind where you fall asleep but don’t get sustained deep sleep) both reduce growth hormone output: the feedback loop needs uninterrupted time to run its full cycle.
As the researchers put it, sleep is not passive downtime between the real business of being awake. It is active, essential biology — the period where the body runs its repair and maintenance programme, and growth hormone is the main tool it uses.
What this means practically: if you train and you’re not sleeping, you are working against yourself in a way that no supplement, no protein intake, and no training programme can fully compensate for. The muscle repair that happens in the gym requires growth hormone. Growth hormone requires deep sleep. That’s the chain. Cutting sleep to make time for more training is one of the more common and counterproductive trade-offs in fitness culture.
The finding is also relevant specifically for women in the luteal phase of the menstrual cycle (the two weeks before a period) where progesterone raises body temperature and fragments deep sleep specifically. During this phase, growth hormone output is lower not because of anything you’re doing wrong, but because the hormonal environment is making it harder to reach and sustain deep non-REM sleep. More sleep time in this phase, cooler sleeping environment, and avoiding alcohol and intense late-evening exercise are the most direct ways to protect the deep sleep that’s being most disrupted.
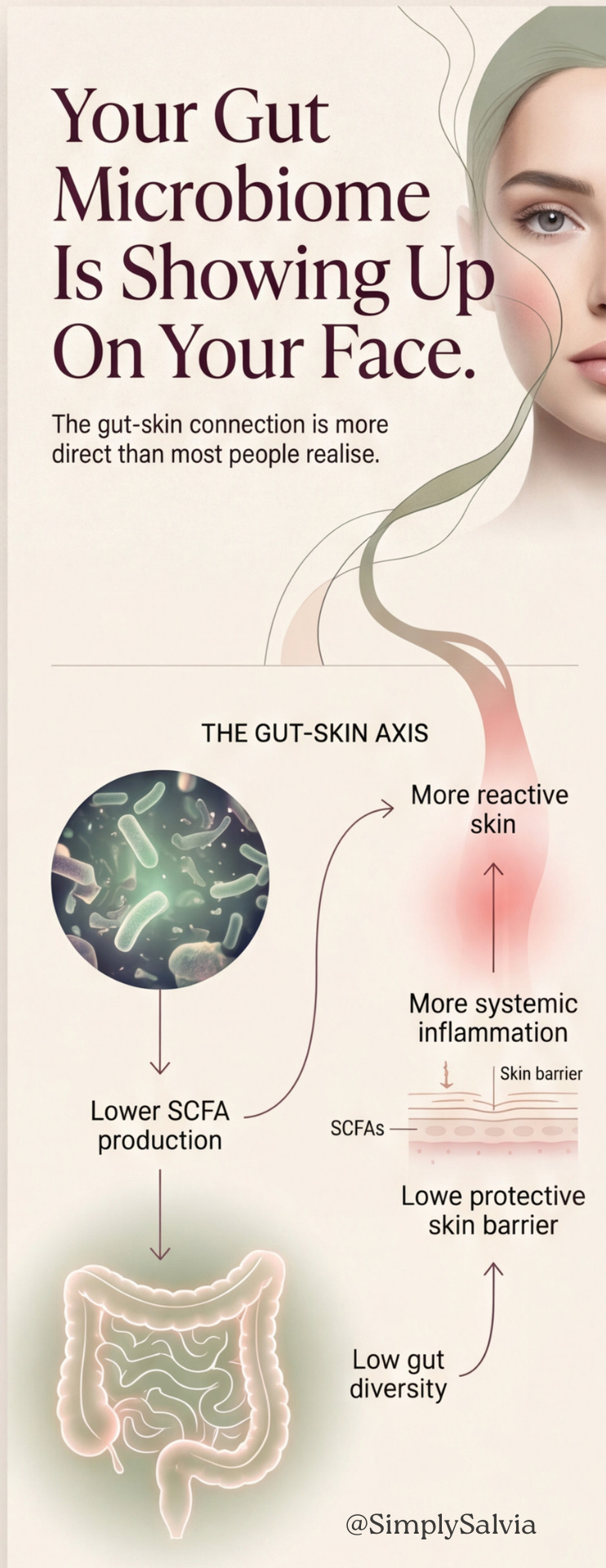
Your Gut Microbiome Is Showing Up On Your Face. The Mechanism Is More Direct Than You Think.
The gut-skin axis (the idea that gut health affects skin health) has been circulating in wellness content for several years. Like most wellness topics that go viral, it’s been both overstated (every skincare problem has a gut cause, take this probiotic) and undersold (the actual mechanism is more interesting than the vague content suggests).
A systematic review published in Microorganisms in December 2025 pulled together the current state of the evidence, covering atopic dermatitis, psoriasis, acne vulgaris, rosacea, chronic urticaria, and melasma, and found that for all of them, there are consistent associations with gut microbiome composition.
The mechanism isn’t a mystery. It runs through several overlapping pathways:
When gut microbiome diversity is low (driven by low-fibre diets, antibiotic use, chronic stress, or poor sleep) the gut produces fewer short-chain fatty acids (SCFAs). SCFAs are the compounds that gut bacteria make when they ferment dietary fibre, and they serve as a primary fuel source and anti-inflammatory signal throughout the body, including in the skin. When SCFA production drops, systemic inflammation rises. Systemically elevated inflammation makes skin more reactive, impairs the skin barrier, and makes inflammatory skin conditions more likely to flare.
The second pathway is direct: the same inflammatory cytokines that circulate when gut dysbiosis is present show up in skin tissue and activate inflammatory cascades there. For acne specifically, research has found that people with acne have measurably different gut microbiome compositions than people without it, and that restoring gut diversity reduces inflammatory acne in a subset of cases.
The third pathway is relevant specifically for hormonal skin issues: the estrobolome (the collection of gut bacteria that metabolise estrogen) regulates how much estrogen is cleared from the body. When gut diversity is low, estrogen clearance is impaired, circulating estrogen rises, and the hormonal acne driven by estrogen dominance worsens. This is the direct route from gut health to jawline and chin breakouts in women.
The practical implication is not that every skincare problem has a gut solution. It’s that for inflammatory skin conditions that aren’t fully responding to topical treatment (persistent acne, rosacea, eczema, reactive or red skin) the gut environment is worth looking at as a contributing factor. The dietary pattern that most consistently supports gut microbiome diversity: high-fibre eating from varied plant sources, fermented foods (kefir, kimchi, yoghurt, sauerkraut), reduced ultra-processed food, consistent sleep, and stress management. None of these are dramatic interventions. Together, they create the conditions in which a diverse gut microbiome can do its job, including the job of keeping your skin less inflamed.
Exercise for Depression and Anxiety Just Got Its Strongest Evidence Yet. The Finding About Type Matters.
There is now more research supporting exercise as a treatment for depression and anxiety than there is for many approved medications. That statement is not an exaggeration.
A systematic umbrella review published in the British Journal of Sports Medicine in February 2026, the most comprehensive analysis of this evidence to date, synthesised 57 pooled data analyses covering 800 individual studies and 57,930 participants. The pooled effect size for exercise on depression was large (standardised mean difference of −0.97). For anxiety, it was medium to large (SMD −0.66). The authors concluded that exercise may be “one of the most powerful treatments” for both conditions, and recommended it as a first-line intervention alongside therapy and medication, not after them.
What this means is worth sitting with: a 2026 review of 800 studies, involving nearly 58,000 people, found that exercise has a large effect on depression. Not a small supportive effect. A large clinical effect comparable to, and in some analyses exceeding — psychological therapy alone.
The finding about type of exercise is the part that matters most for the Simply Salvia audience:
Aerobic exercise, resistance training, and mind-body practices (yoga, tai chi) all showed significant benefits for depression. A separate meta-analysis published in early 2026 found that meaningful clinical improvement in depression and anxiety was observed at exercise volumes well below the WHO weekly guidelines — meaning two short sessions a week produced real effects, and pushing to five sessions a week didn’t add proportionate benefit. The best exercise for mental health is the one you actually keep doing.
There’s also a finding specifically for women: a 2025 study in the Journal of Clinical Medicine found that a resistance training programme significantly reduced depressive symptoms in women, independent of aerobic exercise. The mechanism: resistance training reduces inflammatory cytokines (specifically IL-6 and TNF-alpha), raises BDNF (brain-derived neurotrophic factor, a compound that supports brain plasticity and mood), and produces consistent hormonal changes that support mood regulation. The effect was significant with just two to three sessions per week.
For anyone who’s been in a low period and felt too depleted to exercise: the evidence suggests that starting at a low volume; two sessions per week, moderate intensity produces real and measurable mood effects. The hurdle to get there is real. The effect on the other side of it is also real.
Magnesium: Why Women Are More Deficient, and What the Research Now Says About It
Magnesium is one of the more well-evidenced supplements in the research and one of the most overlooked in general nutrition conversation. A narrative review published in PMC in July 2025, specifically examining sex-based differences in magnesium metabolism found something important: women have lower dietary magnesium intake than men across most populations, and the hormonal fluctuations of the menstrual cycle create additional demand for magnesium that isn’t reflected in the standard recommended daily intake.
Why does this matter? Because magnesium is involved in over 300 enzymatic reactions in the body. The ones most relevant for women specifically:
GABA receptor activation. Magnesium activates the GABA-A receptor system, the same system that progesterone’s metabolite activates, and the same system that targeted by anxiety medications. When magnesium is low, GABA support is lower, the nervous system is more excitable, and anxiety, restlessness, and difficulty sleeping all increase. When magnesium falls (as it does in the late luteal phase, when progesterone drops), the GABA gap widens. Supplementing magnesium in the late luteal phase partially fills this gap.
PMS symptom reduction. Research has consistently found that 300mg of magnesium daily reduces PMS symptoms, specifically bloating, mood changes, and anxiety. A 2026 guide from Mito Health noted that combining 300mg magnesium with 30mg B6 reduces PMS symptoms by approximately 60%, because B6 amplifies magnesium’s absorption at the cellular level and independently supports serotonin and GABA synthesis.
Muscle relaxation and cramping. Magnesium relaxes smooth muscle including uterine smooth muscle. This is the mechanism behind its effect on menstrual cramping. It also explains why magnesium deficiency is associated with more severe cramping: the muscle is less able to relax between contractions.
Blood sugar regulation. Magnesium is required for insulin receptor function. Low magnesium is associated with insulin resistance which creates worse blood sugar instability, which drives the energy crashes and carbohydrate cravings of the luteal phase. Correcting magnesium deficiency supports insulin sensitivity and smooths the blood sugar rollercoaster that makes the premenstrual week harder.
Sleep quality. Magnesium activates GABA, which is why it promotes the nervous system calm that supports sleep initiation. Magnesium glycinate specifically (the form with highest bioavailability for neurological effects) has the most consistent evidence for improving sleep quality and reducing sleep onset time.
The standard blood test for magnesium (serum magnesium) only measures about 1% of the body’s total magnesium stores and is notoriously unreliable for detecting true deficiency. This means you can test as “normal” and still be functionally deficient. Symptoms of low magnesium; fatigue, irritability, muscle cramps, poor sleep, PMS, are also the symptoms most commonly attributed to stress or “just being a woman.” They are worth taking seriously.
The information in this post is for educational and informational purposes only. None of the above constitutes medical advice. Always consult a qualified healthcare professional for personal health concerns.
Between Saturdays is a weekly research roundup from Simply Salvia. Four things from science and wellness worth knowing about. If someone sent this to you, you can subscribe here.