Between Saturdays: What's Actually Happening Inside Your Body Right Now
From the plastic particles found inside human ovaries, to the supplement nobody told women about, to why your anxiety might start in your stomach. Four things quietly happening in your body.
You can’t feel any of this happening.
That’s the part that struck me most when I pulled the research for this week’s post. Not that it’s alarming, though some of it is but that it’s invisible. The plastic particles are too small to feel. The bacteria shaping your mood are doing it through pathways you never think about. The supplement that’s been studied for decades for men’s athletic performance is only just being investigated in women’s brains. The thing that’s burning out your nervous system looks, from the outside, like a completely ordinary Tuesday.
This week I wanted to look at four things that are happening inside people’s bodies right now, whether they know it or not and what, if anything, the research actually tells us to do about it.
Caught My Eye…
The Plastic Particles Inside Human Ovaries
In February 2025, a team of Italian researchers published what they described as a first: evidence of microplastic particles in human ovarian follicular fluid; the liquid that surrounds a developing egg before ovulation. It was the first time anyone had confirmed their presence there.
The study was small with a total of 18 women undergoing IVF treatment at a clinic in Salerno, but the findings were striking. Microplastic particles smaller than 10 micrometers were detected in 14 of the 18 follicular fluid samples, with an average concentration of 2,191 particles per millilitre. These are particles small enough to cross cellular membranes. They entered through the bloodstream and reached the granulosa cells surrounding the egg.
The researchers also found something that deserves more attention than it has received: a significant correlation between microplastic concentration in the follicular fluid and levels of Follicle-Stimulating Hormone (FSH). Elevated FSH can indicate reduced ovarian reserve. One of the key markers used to assess a woman’s fertility potential. The study didn’t establish causation, and the researchers were careful to note that no direct correlation was found with fertilisation outcomes or live birth rates. But the signal is there, and it’s the first time anyone has looked.
This finding doesn’t exist in isolation. A 2024 scoping review published in the Journal of Global Health found that microplastics have now been detected in 8 out of 12 human organ systems, including the cardiovascular, digestive, endocrine, reproductive, and urinary systems. They have been found in breast milk, in the placenta, in the lungs, the liver, the kidneys, the colon, and, as a study published in Nature Medicine in early 2025 confirmed, in human brain tissue — at concentrations roughly 50% higher in 2024 samples than in samples from 2016. Researchers found that brain tissue samples from cognitively normal individuals averaged 4,800 micrograms per gram, the equivalent of an entire plastic spoon by weight.
We are at the beginning of understanding what this means. The mechanisms are not fully mapped, and researchers are cautious about drawing firm conclusions from what is still an emerging field. What is clear is that microplastics primarily enter the body through ingestion, inhalation, and skin contact, with traces now found across a broad range of human tissues and biological fluids. The exposure is ongoing. It is not avoidable, but it is reducible: glass or stainless steel water bottles over plastic, not microwaving food in plastic containers, swapping synthetic clothing for natural fibres where possible. These are not solutions. But they matter at the margins, and the margins are where individual exposure can be reduced while the larger regulatory and industrial questions are fought out.
Your Gut Is Producing Your Mood And You’re Probably Feeding It Wrong
You have likely heard that gut health matters. What the research is now showing is how specifically and mechanistically it matters, in ways that go well beyond digestion.
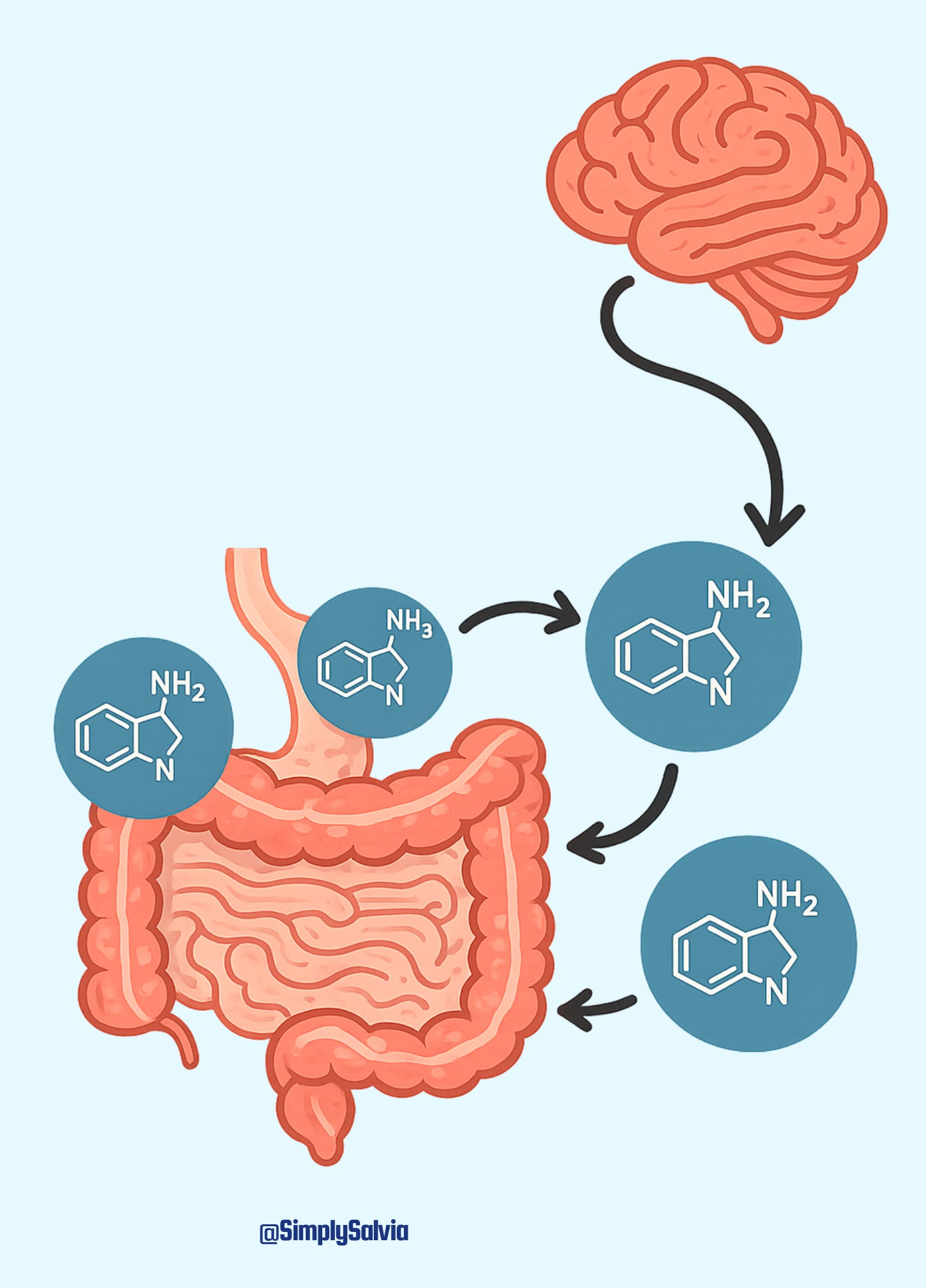
The gut-brain axis is a bidirectional communication network between your gastrointestinal system and your central nervous system, mediated by the vagus nerve, the immune system, and the hormones your gut produces. Disruptions in gut microbiota composition may trigger or exacerbate symptoms of anxiety and depression by interfering with these communication pathways, including neural signalling through the vagus nerve, hormone regulation through the HPA axis, immune responses involving pro-inflammatory cytokines, and metabolic processes related to short-chain fatty acids.
Here is the part that most people don’t know: gut microbiota produce and regulate serotonin, dopamine, and GABA aka the key neurotransmitters involved in mood, emotional regulation, and anxiety. Around 90% of the body’s serotonin is produced in the gut, not the brain. The bacteria you’re hosting are not just processing food. They are producing the chemical environment of your emotional life.
A large-scale genome-wide association study published in Nature Communications, involving over 1,000 participants from the Rotterdam Study cohort and nearly 1,600 from a separate validation cohort, identified thirteen microbial taxa associated with depressive symptoms, including bacteria known to be involved in the synthesis of glutamate, butyrate, serotonin, and GABA. This wasn’t a correlation with lifestyle or diet in the conventional sense. It was a specific mapping of which bacterial species track with depression and which are absent in people who have it.
One of the most compelling pieces of evidence for causality came from a study by neurobiologist John Cryan at University College Cork. His team took microbiome samples from people with depression and transplanted them into healthy rats. The rats developed depression-like behaviours; anhedonia, anxiety, and altered tryptophan metabolism, suggesting the microbial community itself was driving the mood changes, not merely reflecting them.
The practical implications are still being worked out. Probiotics show promise but the research is not yet at the point of specific prescriptions. What is better established: a diet high in diverse plant foods, fibre, fermented foods, and omega-3 fatty acids supports microbial diversity, and microbial diversity is consistently associated with better mental health outcomes. Ultra-processed food, chronic stress, sleep deprivation, and antibiotics all deplete it. The gut is not separate from mental health. It is, increasingly, part of the same system.
Creatine: The Supplement Nobody Told Women About
If you follow fitness content, you’ve heard of creatine. You probably also absorbed, somewhere along the way, the idea that it’s a bodybuilder’s supplement — something for men trying to build muscle, not particularly relevant to you.
That assumption is being quietly dismantled by a growing body of research that has almost nothing to do with muscle.
Creatine is a naturally occurring compound that your body synthesises from amino acids, and that you get in small amounts from red meat and fish. Its primary role is in the phosphocreatine energy system, a fast-access energy pathway used heavily by muscles during intense exercise. But the same system operates in the brain. Your neurons use phosphocreatine to regenerate ATP during periods of high cognitive demand, and when brain creatine stores are depleted — by sleep deprivation, mental fatigue, stress, or simply the natural variation in creatine synthesis, cognitive performance drops.
There is emerging interest in the potential beneficial effects of creatine supplementation on brain health and function. Creatine supplementation can increase brain creatine stores, which may help explain some of the positive effects on measures of cognition and memory, especially in ageing adults or during times of metabolic stress such as sleep deprivation.
A 2024 meta-analysis published in Frontiers in Nutrition, reviewing randomised controlled trials spanning three decades, found that creatine supplementation showed meaningful cognitive benefits particularly under conditions of metabolic stress — sleep deprivation, mental fatigue, hypoxia. For women specifically, the picture is more complicated and less studied: whether any sex or age-related differences exist in regard to creatine and brain health is relatively unknown, because most of the trials have enrolled predominantly male participants.
What we do know is that women have naturally lower creatine stores than men, synthesise less of it endogenously, and experience significant fluctuations tied to the menstrual cycle particularly during the luteal phase, when energy demands increase and cognitive performance often dips. A 2025 clinical trial specifically enrolling perimenopausal and menopausal women found promising early results for creatine’s effects on brain creatine levels and cognitive resilience, though the authors noted that larger trials are needed before firm conclusions can be drawn.
The honest nuance: a key uncertainty is whether supplemented creatine crosses the blood-brain barrier in sufficient amounts to affect neuronal metabolism, and assertions of cognitive enhancement based solely on supplementation risk overstating available data. This is a field that is moving fast, but has not yet arrived at clinical consensus. Creatine is safe and well-studied for physical performance. Its brain effects are real but not yet fully quantified. If you’re already taking it for training, there is a reasonable case that your brain may also benefit, particularly on difficult cognitive days. If you’re not, it’s not yet evidence-based enough to recommend as a cognitive supplement for women specifically but the research is getting there, and getting there quickly.
Your Nervous System Is Exhausted And It’s Not the Same Thing as Being Tired
The last one doesn’t have a single landmark study. It has hundreds. And it’s the one your body is probably the most familiar with, even if you’ve never had language for it.
Nervous system dysregulation — sometimes called chronic sympathetic dominance, or persistent activation of the fight or flight response, is a state in which the autonomic nervous system gets stuck in high alert. Not because there is an emergency. But because the modern environment, for a lot of people, never stops signalling that there might be.
When the sympathetic nervous system remains chronically activated, such as in cases of ongoing stress or trauma, it can lead to cardiovascular problems, digestive disorders, immune system dysfunction, anxiety, and depression. Chronic sympathetic arousal can also impair the body’s ability to heal and repair itself as in a state of constant vigilance, resources are diverted away from maintenance and restoration towards immediate survival needs.
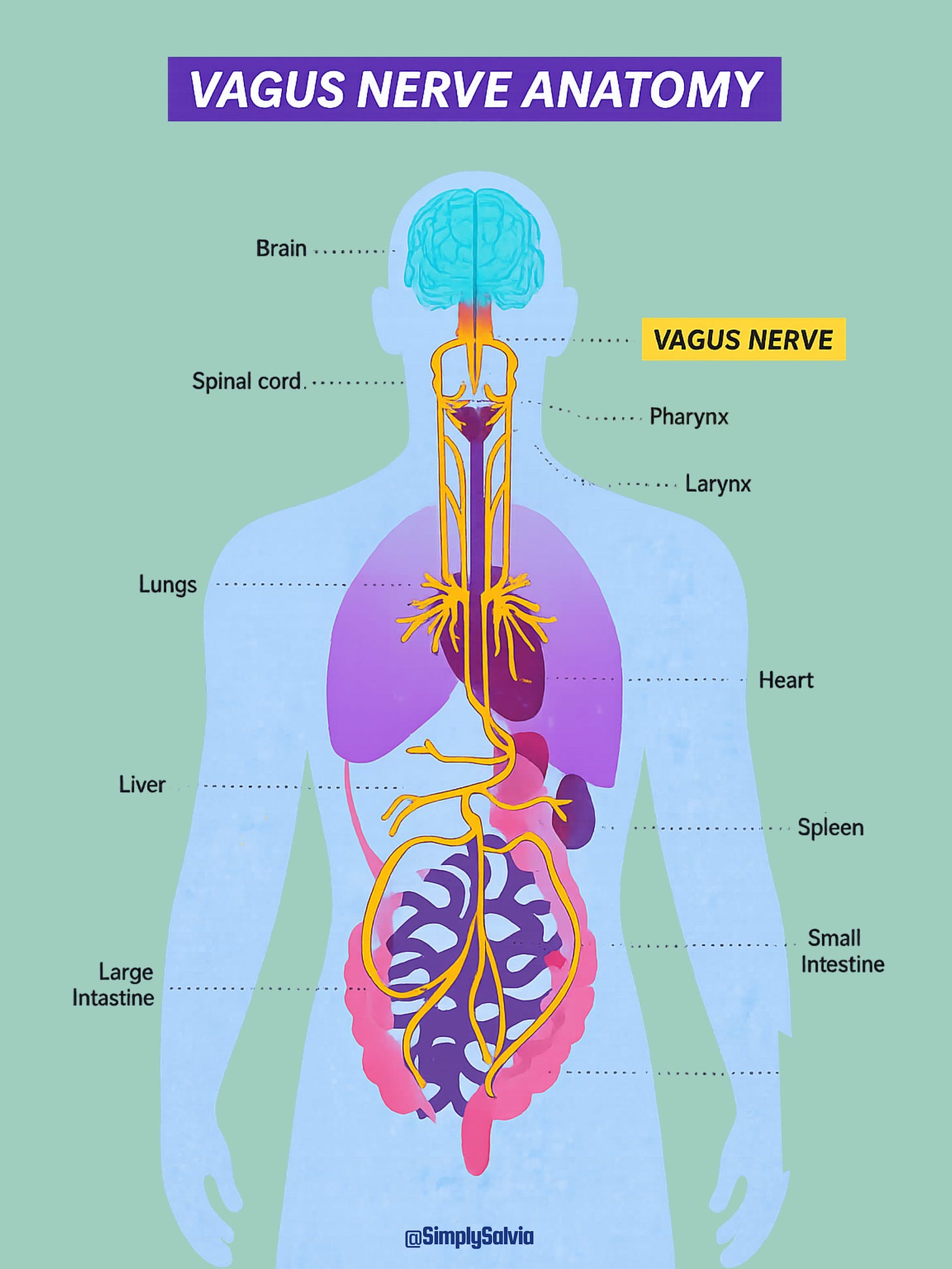
The vagus nerve is at the centre of the emerging science on how to regulate this. It is the longest cranial nerve in the body, running from the brainstem to the abdomen and connecting most of the major organs along the way. It is the primary nerve of the parasympathetic system aka the rest and digest counterpart to fight or flight. Decades of research have established a critical role for vagus nerve signalling in emotional regulation, cognitive performance, inflammation response, and physical recovery.
Crucially, vagal tone — the baseline activity of the vagus nerve is not fixed. It can be trained. Cross-sectional studies in healthy adults repeatedly show that higher vagal tone, measured by heart rate variability, tracks with superior executive performance, sustained attention, and working memory. And the practices that increase vagal tone are unglamorous but real: slow diaphragmatic breathing, cold water exposure to the face and neck, humming, singing, exercise, social connection, and adequate sleep. These are not wellness trends. They are physiologically grounded inputs into a system that a significant number of people are running on depleted.
A 2024 pilot study published in Frontiers in Neurology found that transcutaneous vagus nerve stimulation, a non-invasive form applied through the ear improved symptoms in a female cohort with Long COVID, a condition characterised in part by autonomic nervous system dysfunction. The study was small and preliminary. But it points toward the same conclusion that the broader research base is converging on: the nervous system is not a fixed background condition. It is responsive, trainable, and more central to overall health than most people are taught to think.
The question worth sitting with is not whether you are stressed. Most people reading this know they are. The question is whether your nervous system has had enough consistent input, enough moments of genuine, physiological safety to come back down between the stressors. For most people living with overfull schedules, screens, poor sleep, and chronic low-level anxiety, the honest answer is probably no. That’s not a personal failing. It is a mismatch between the nervous system’s evolutionary design and the environment it is currently trying to survive.
Source: Tyler, Frontiers in Psychology, 2025. Zheng et al., Frontiers in Neurology, 2024. MDPI Neuroimmune Review, December 2025.
In Summary
Four things happening in your body right now that most people don’t know about:
→ Microplastic particles have been found in human ovarian follicular fluid for the first time, at an average of 2,191 particles per millilitre. They’ve also been found in brain tissue, the placenta, lungs, liver, and blood. The science is still early. The exposure is real and ongoing. Reducing plastic in food and drink contact is the most practical lever available.
→ Your gut microbiome is producing serotonin, dopamine, and GABA — the neurotransmitters that shape your mood. Specific bacterial species are now linked to depression and anxiety at a mechanistic level. Microbial diversity, supported by a varied plant-rich diet, is increasingly understood as a component of mental health, not just digestion.
→ Creatine has cognitive benefits that most women don’t know about, particularly under conditions of sleep deprivation and mental fatigue. Women have lower natural creatine stores than men, and the research into sex-specific cognitive effects is only just beginning. Promising, but not yet at clinical recommendation stage for women specifically.
→ Nervous system exhaustion is not the same thing as being tired. Chronic activation of the fight-or-flight response has measurable effects on immunity, digestion, cognition, and emotional regulation. Vagal tone is trainable. Slow breathing, exercise, sleep, and genuine rest are physiological inputs — not indulgences.
The information in this post is for educational purposes only and does not constitute medical advice. If you have concerns about any of the topics covered here, please consult a qualified healthcare professional.
Detailed Readings
Gut Microbiome-Wide Association Study of Depressive Symptoms — Nature Communications, 2022
Why Nurturing the Gut Microbiota Could Resolve Depression and Anxiety — Nature, 2025
Heads Up for Creatine Supplementation and Brain Health — PMC
The Vagus Nerve: A Cornerstone for Mental Health and Performance — Frontiers in Psychology, 2025