Between Saturdays: What Your Nails Are Trying to Tell You
From the dark streak that gets misdiagnosed for years, to the myth that's convinced an entire generation they need zinc supplements. Your nails are recording your health history. Are you reading them?
Go look at your nails right now.
Not to see if they need a file. Not to check your polish. Look at them the way a doctor would — the colour, the shape, the texture, the lines. Because your nails aren’t just keratin. They’re a slow-moving record of everything your body has been through over the past six months: the illness, the stress, the deficiencies, the things your blood work might not have caught yet.
In this edition of Between Saturdays, I’am going through four things your nails might be telling you right now, including one that gets misdiagnosed for an average of ten years, and one that most of the internet has completely wrong.
Let’s get into it.
Caught My Eye…
The Dark Streak That Gets Ignored For Years
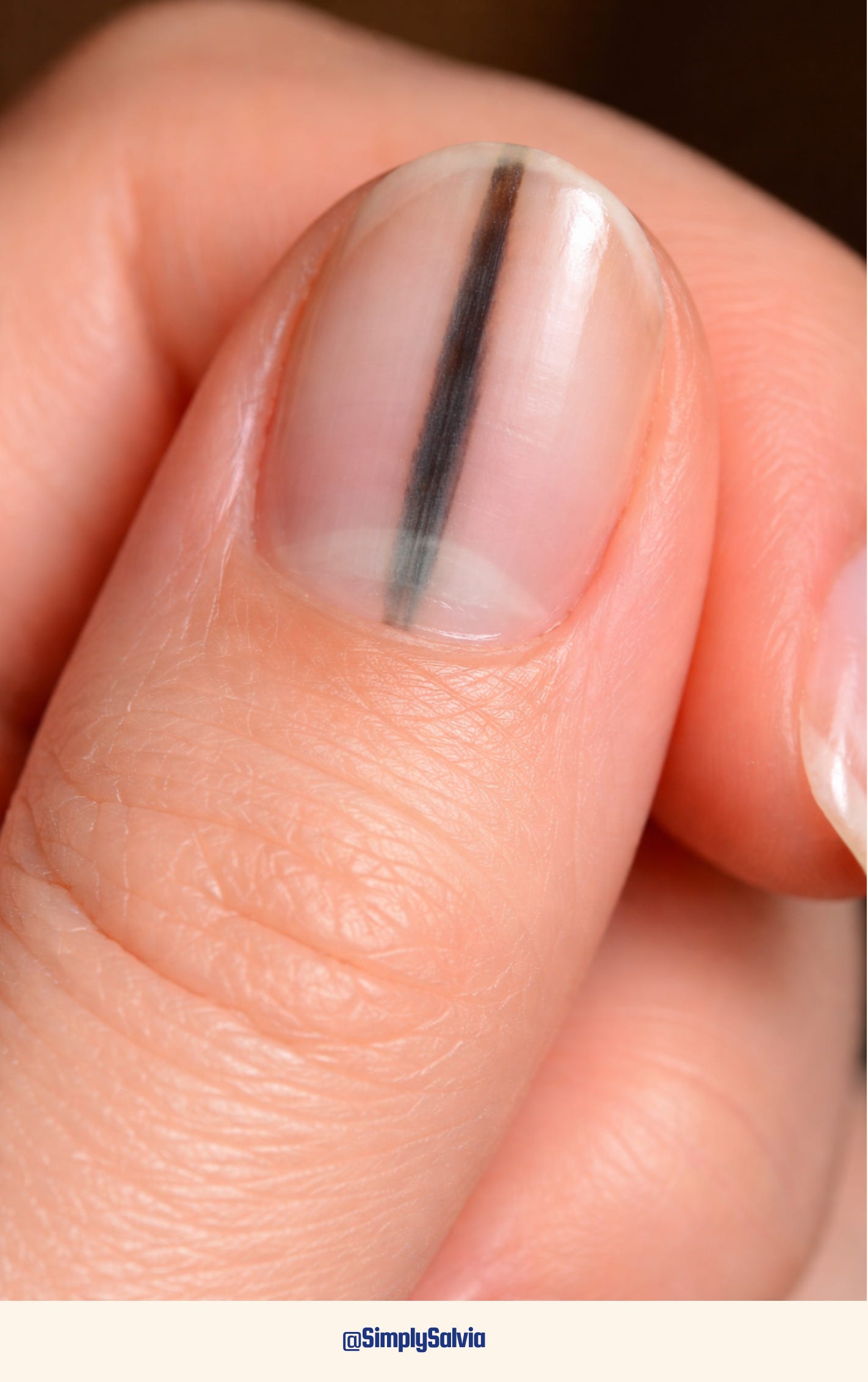
Most people, if they noticed a dark vertical streak running down one of their nails, would assume it was a bruise. They’d wait for it to grow out. They’d forget about it.
That assumption has cost lives.
A dark longitudinal band under the nail — a line running from the base to the tip, brown or black in colour is the most common presenting sign of subungual melanoma: a rare but serious cancer that develops under the nail.
Unlike other melanomas, it has no connection to UV exposure. It doesn’t come from sunbathing or tanning beds. It can develop on anyone, at any age, regardless of skin tone. In fact, among people with darkly pigmented skin, subungual melanoma accounts for up to 30% of all melanoma diagnoses — making it disproportionately common in Black, Asian, and Hispanic populations.
The reason outcomes are often so poor is not because the cancer is inherently untreatable. It’s because it is almost universally diagnosed late. A 2019 study found that the average time from the appearance of a pigmented nail lesion to biopsy was more than ten years. Ten years of being told it was a bruise, a fungal infection, a harmless pigmentation. In most cases by the time a histologic diagnosis is made, the lesion is already deep. The 5-year survival rate when caught early sits around 97%. When caught late, it drops to between 15–20%.
This is a cancer where the difference between early and late diagnosis is the difference between a minor procedure, losing a digit or worse.
The warning signs to know: a dark band wider than 3mm, a band that is triangular in shape (wider at the base than at the tip), irregular or blurred edges, pigment that spreads onto the surrounding skin at the base of the nail, or a band that appeared recently and is growing. Dermatologists use an ABCDEF rule for subungual melanoma specifically:
Age,
Band characteristics,
Change in the nail,
Digit involved,
Extension of pigment, and
Family history.
Any band that you can’t explain with a specific remembered injury, or that is changing, is worth having assessed by a dermatologist promptly.
Take your nail polish off before your next skin check. Ask your GP or dermatologist to look.
Your Nails Recorded Your Illness — Even If You Didn’t Know You’d Had One
If you ever had COVID-19, or a serious fever, or a period of extreme physical stress, there is a chance your nails quietly recorded it — weeks or months after the fact.
Beau’s lines are horizontal grooves that run across the width of the nail. They form when the nail matrix aka the tissue at the base of the nail responsible for producing new growth temporarily slows down or stops completely. The nail keeps growing, but there’s a gap where it paused: a transverse dent in the plate that moves outward as the nail grows, like a ring on a tree.
A 2024 systematic review published in Pathogens found significant evidence linking Beau’s lines to COVID-19 infection, particularly severe cases requiring hospitalisation. The lines typically appear two to three weeks after the systemic insult, and their distance from the nail fold can be used to estimate roughly when the illness occurred — fingernails grow at approximately 2–3mm per month, so a groove sitting 6mm from the proximal fold means the event happened around two months ago.
But COVID-19 is just one trigger. Beau’s lines can follow any significant physiological disruption: severe febrile illness, chemotherapy cycles, extreme malnutrition, Kawasaki disease, major surgery, or acute emotional trauma — a death, a breakdown, a prolonged period of severe stress. Essentially, when the body reaches a triage situation, it stops building nails and redirects resources. The groove that appears weeks later is the physical receipt.
As one Cleveland Clinic dermatologist put it: your body was preoccupied, and growing nails is much lower on the priority list when you’re extremely sick.
The lines are harmless and will grow out. But if you notice a horizontal groove across multiple nails that you can’t explain by local trauma, it’s worth thinking back over the past two to three months and considering whether your body went through something significant, even something you thought you recovered from.
White Spots: The Myth That Won’t Die
If you’ve ever had white spots on your nails, you were almost certainly told one of these things: you’re low in calcium, you’re low in zinc, or you’re not absorbing vitamins properly.
You were almost certainly wrong — and so was whoever told you.
A study published in the Journal of Human Nutrition and Dietetics set out specifically to test this belief. Researchers surveyed 82 university students, measured their calcium and zinc intake scores using a validated food frequency questionnaire, and counted the white spots on their nails. The result: there was no statistically significant association between white spots and calcium intake, zinc intake, age, gender, hand dominance, or multivitamin use. The only factor that correlated with white spots was one variable: how frequently participants engaged in activities that knocked their hands.
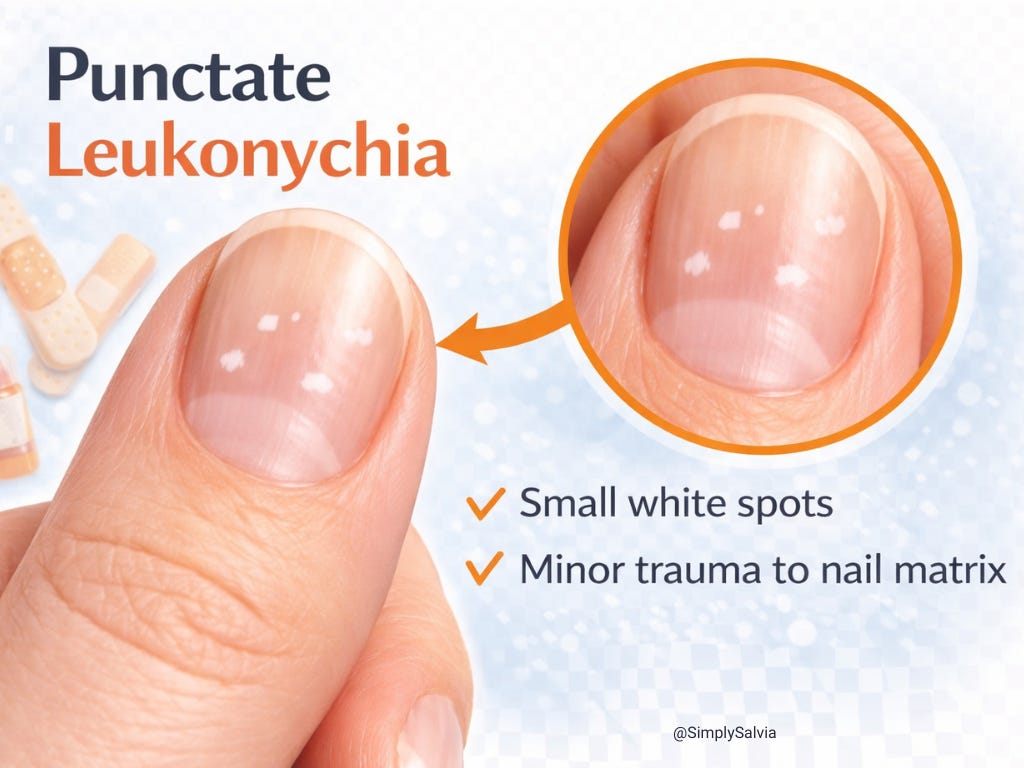
Punctate leukonychia — the small white spots most people get is, in the overwhelming majority of cases, minor trauma to the nail matrix. The matrix sits beneath the skin at the base of your nail, and it doesn’t take much to disrupt it: an aggressive manicure, bumping your hand, pressing on your cuticles, wearing tight rings. The disruption happens, you don’t notice it, and two to six weeks later the spot emerges as the nail grows out. By the time you see it, the event that caused it is long forgotten.
The zinc-deficiency myth, in particular, has taken on a life of its own — spread by wellness influencers, supplement brands, and the kind of content that tells you every physical complaint is a nutritional deficiency you need to buy your way out of. According to the PMC review Leukonychia: What Can White Nails Tell Us?, punctate leukonychia
“is not related to reduced calcium or iron content of the nail plate, as popularly believed. Usually, it is due to trauma.”
That said, nuance matters. If your white spots are persistent, spreading, involve the entire nail, or are accompanied by nail thickening, brittleness, changes in skin or hair, or other symptoms, they can occasionally point to fungal infections, psoriasis, or in rarer cases, systemic conditions. Zinc deficiency can cause leukonychia, but typically in severe, chronic deficiency and not the garden-variety kind your supplement brand is marketing to you.
The rule of thumb: isolated, small white spots that move as your nail grows are almost always old trauma, not a deficiency. Recurring spots across multiple nails with other symptoms are worth getting checked.
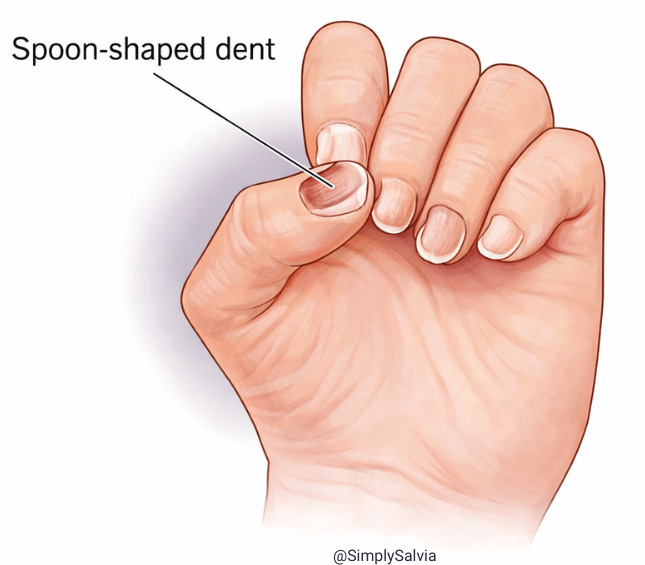
Spoon-Shaped Nails: When Your Body Has Run Out of Iron
The last one is quieter and more common than most people realise, especially in women.
Koilonychia is the medical term for nails that have lost their normal curve and become flat, then concave — literally scooped out, like the bowl of a spoon. In early stages, nails may just seem unusually flat or brittle, prone to splitting at the tips. As it progresses, the nail plate becomes visibly depressed in the centre and raised at the edges, sometimes enough that a water droplet placed on the nail will hold its shape rather than rolling off.
The most common cause is chronic iron deficiency anaemia. Iron deficiency is the commonest nutritional cause of anaemia worldwide, and it is considerably more prevalent in women of reproductive age — a combination of menstrual blood loss, dietary patterns, and the fact that iron deficiency frequently goes unrecognised and untreated for years before it reaches the point of anaemia. The nail changes aren’t caused by the anaemia itself but by iron depletion at a cellular level. Reduced iron in the iron-containing enzymes of epithelial cells weakens the connective tissue beneath the nail plate, causing it to deform under mechanical pressure.
A case report published in The American Journal of Medicine documented a patient whose spoon nails resolved entirely after 16 weeks of oral iron supplementation, demonstrating that the deformity is reversible when the underlying deficiency is addressed.
The reason this matters for our age group specifically: iron deficiency is common, it’s underdiagnosed, and its symptoms are often attributed to burnout, poor sleep, or stress. Fatigue, cold hands and feet, brain fog, brittle nails, hair thinning, pale inner eyelids — these are all signs that can be easy to explain away. Koilonychia is a physical sign that the deficiency has been going on long enough to change the structure of your nails.
If your nails are flattening or beginning to look concave, it’s worth asking your GP for a full iron panel and not just haemoglobin, but ferritin and transferrin saturation. You can be functionally iron deficient with a haemoglobin level that looks normal.
In Summary
Four things your nails might be recording right now:
→ A dark vertical streak is not automatically a bruise. It could be subungual melanoma, a cancer with a 97% survival rate when caught early, and a 15–20% rate when caught late. Average time to diagnosis: ten years. Take your polish off and look.
→ Horizontal grooves (Beau’s lines) are your body’s receipt for a stressful event: an illness, a fever, chemotherapy, extreme stress. They appear 2–3 weeks after the event and can be used to date roughly when it occurred.
→ White spots are almost always old trauma from knocking your nail matrix. The zinc and calcium deficiency myth has no solid research behind it. Isolated small spots that move as the nail grows are harmless. Persistent, spreading spots with other symptoms are worth checking.
→ Concave, spoon-shaped nails (koilonychia) are a physical sign of chronic iron deficiency — common in women of reproductive age, often missed because the symptoms look like burnout. Reversible with treatment. Ask for a ferritin test, not just haemoglobin.
The information in this post is for educational purposes only and does not constitute medical advice. If you notice any concerning nail changes, please consult a qualified healthcare professional or dermatologist. Do not self-diagnose based on nail appearance alone.
Detailed Readings
Subungual Melanoma — StatPearls, NCBI Bookshelf
Beau’s Lines and COVID-19: A Systematic Review — Pathogens, 2024
Koilonychia in Iron Deficiency Anaemia — American Journal of Medicine, 2022