Between Saturdays: What Stress Is Actually Doing
Four patterns in the body you’ve felt, but probably never connected.
This edition is about stress, not as a feeling, but as a biological pattern. The kind that shows up across systems: in the heart, the immune response, sleep, and the way the mind interprets experience itself.
What’s striking, once you look at the research side by side, is not just that stress affects everything. It’s that it does so through predictable pathways. And those pathways explain why stress feels the way it does and why it accumulates in ways that are easy to dismiss until they’re not.
Caught My Eye…
Stress and the Heart: The Risk That Builds Without Symptoms
There’s a version of cardiovascular risk that doesn’t feel like risk.
A large pooled analysis of nearly 200,000 individuals looked at what happens when people live under sustained job strain; high demand, low control. Over time, those individuals had a 23% higher risk of developing coronary heart disease.
Not dramatically higher. But consistently higher. And importantly, higher even after accounting for the usual explanations like smoking, weight, socioeconomic factors.
The mechanism is not a single trigger. It’s repetition.
Chronic stress keeps the body in a state of low-grade activation:
Cortisol remains elevated longer than it should
Blood pressure resets slightly higher
Inflammatory signaling becomes more persistent
The autonomic nervous system leans sympathetic instead of balanced
None of these changes are extreme enough to notice day-to-day. But over years, they alter the baseline the heart operates within.
The important shift here is conceptual: stress is not just an emotional experience. It becomes a physical environment the cardiovascular system has to function inside.
The Immune System: Why Stress Can Help — Until It Doesn’t
Stress is not inherently harmful.
A meta-analysis spanning over 300 studies shows that acute stress, the short-lived kind, actually enhances certain immune functions. It mobilizes immune cells, increases inflammatory readiness, and prepares the body for potential injury or infection.
This is the stress response working exactly as designed.
But the system is built on a cycle: activation, then recovery.
When stress becomes chronic, the recovery phase disappears. And the immune system shifts in a different direction entirely.
Instead of heightened readiness, you see:
Suppressed cellular immunity
Reduced antibody responses
Impaired ability to regulate inflammation
The system doesn’t stay “on.” It becomes dysregulated.
This explains something people often notice but don’t connect: why periods of prolonged stress are often followed by getting sick, slower recovery, or persistent low-level fatigue. The immune system hasn’t failed — it’s been operating without reset.
Stress and Sleep: When the Body Refuses to Power Down
Sleep is where stress becomes visible.
In a large longitudinal analysis designed to approximate a trial, researchers tracked how changes in job strain influenced sleep over time. When stress increased, the likelihood of developing new insomnia symptoms rose significantly. When stress decreased, those symptoms were less likely to persist.
What this shows is direction.
Sleep disruption isn’t random, and it isn’t purely behavioural. It is often a direct reflection of physiological arousal that hasn’t resolved.
Under chronic stress, the body struggles to transition into the state sleep requires:
Cortisol remains elevated later into the evening
Sympathetic nervous system activity stays higher
The usual “drop” in arousal that initiates sleep is blunted
The result is familiar: difficulty falling asleep, fragmented sleep, waking without feeling restored.
The key detail here is that when stress changes, sleep follows. The system is still responsive, it’s just responding to the signal it’s being given.
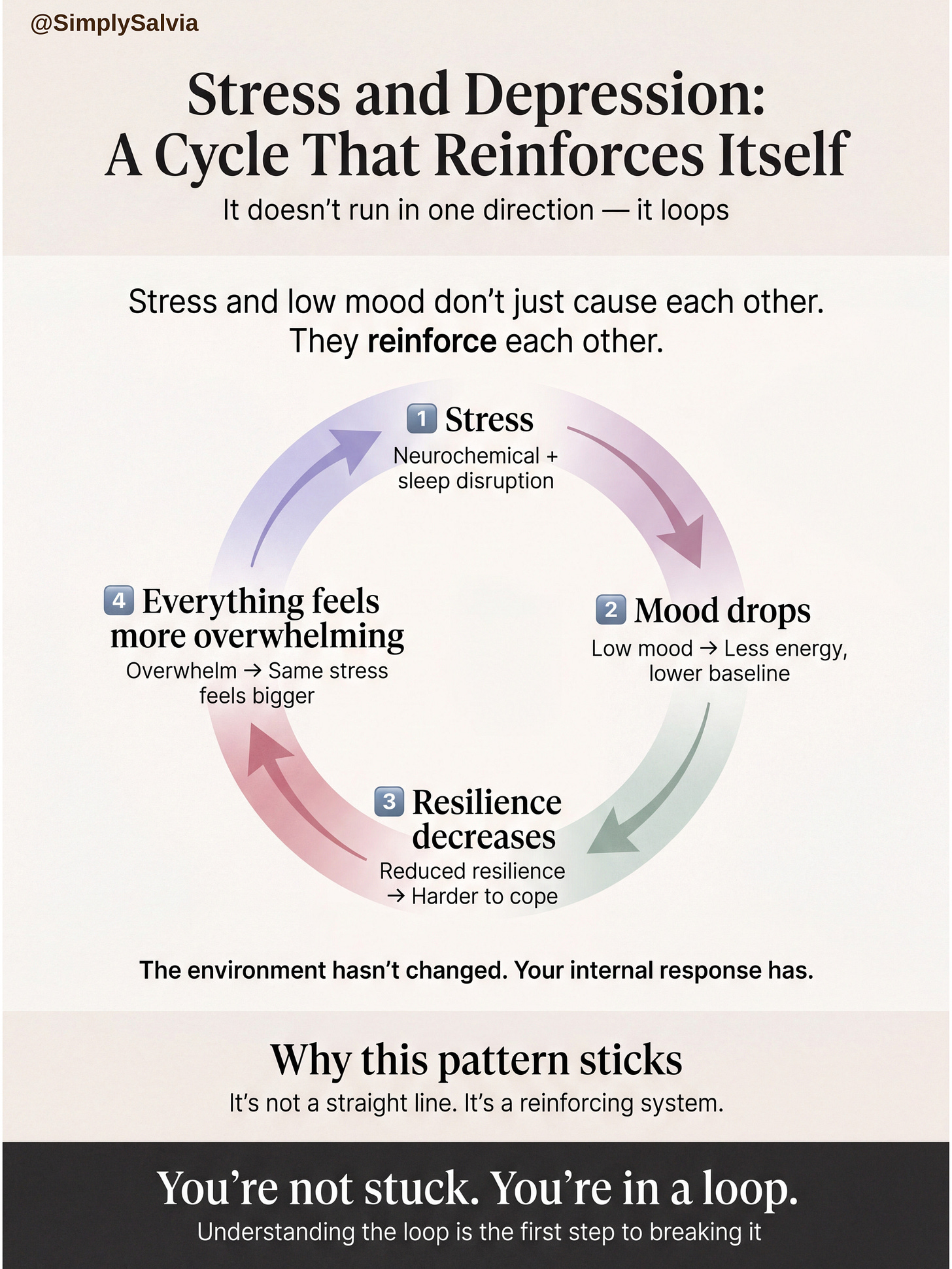
Stress and Depression: A System That Feeds Itself
One of the most persistent misconceptions about stress and mental health is that the relationship runs in one direction.
This creates a feedback loop.
Stress lowers mood by altering neurotransmitter balance, sleep, and energy regulation.
Lower mood reduces resilience and increases cognitive load.
Reduced resilience makes the same external demands feel more overwhelming.
The environment hasn’t changed. The internal response has.
This is why stress-related mental health patterns often feel difficult to break. They are not a straight line from cause to effect. They are a system reinforcing itself from both directions.
The information in this post is for educational and informational purposes only. None of the above constitutes medical advice. Always consult a qualified healthcare professional for personal health concerns.
Between Saturdays is a weekly research round-up from Simply Salvia. Four things from science and wellness worth knowing about. If someone sent this to you, you can subscribe here.
Detailed Readings:
Work stress can raise risk of heart attack by 23%, study finds
Immunology of Stress: A Review Article
Change in Job Strain as a Predictor of Change in Insomnia Symptoms